blog spot
THE
health hub
A collection of helpful articles & information to spread awareness through education from our staff to you
Recent public health reports confirm that measles cases are increasing again in parts of the United States. While outbreaks may not be widespread in every region, the virus’s ability to spread rapidly makes vaccination status an important topic for families in Manassas.
The most effective protection remains full immunization with the MMR vaccine.

Understanding the Risk
Measles spreads through the air and can infect individuals who were never in direct contact with a sick person. Because symptoms initially resemble a routine viral illness, measles can circulate for days before being identified.
Early symptoms often include high fever, cough, runny nose, and red eyes. The rash appears later. By that point, a child may already have exposed others.
Although many children recover, complications can include pneumonia, dehydration, ear infections, and in rare cases, brain inflammation. Hospitalization is not uncommon in outbreak settings.
These risks are significantly reduced in vaccinated children.
It is common for parents to have questions about vaccine safety. The MMR vaccine has been extensively studied worldwide and continues to be monitored for safety. Side effects are generally mild and temporary, such as soreness at the injection site or a low-grade fever.
If you have concerns, discussing them with a pediatric provider allows for informed decision-making based on evidence rather than misinformation.
If your child is due for an MMR vaccine in Manassas, now is the time to confirm protection.
How Effective Is the MMR Vaccine?
The MMR vaccine protects against measles, mumps, and rubella. For measles specifically:
• One dose is approximately 93 percent effective
• Two doses are approximately 97 percent effective
That level of protection is considered extremely strong in preventive medicine. For most children who receive both recommended doses, immunity is long-lasting.
The standard schedule recommended by the CDC is:
• First dose between 12 and 15 months
• Second dose between 4 and 6 years
If your child has received both doses, they are highly protected. If you are unsure, this is the time to review records.
Is the Measles (MMR) Vaccine Safe for Children?
Safety is often the first concern for families in Manassas considering immunizations. The MMR vaccine is one of the most extensively studied vaccines in pediatric medicine.
Before approval, vaccines must pass through:
• Pre-clinical laboratory testing
• Phase 1, 2, and 3 clinical trials
• FDA review
• Ongoing post-licensure monitoring
Even after decades of use, safety monitoring continues through national reporting systems.
The vast majority of children tolerate the MMR vaccine without issue. When side effects occur, they are generally mild and short-lived, including:
• Temporary soreness at the injection site
• Low-grade fever
• Mild rash
Severe allergic reactions are extremely rare.
Extensive research has shown no association between the MMR vaccine and autism. Multiple international studies have confirmed its safety profile.
From a medical standpoint, the risk of measles infection — including complications like pneumonia or encephalitis — far outweighs the risk of vaccine side effects.
For families searching for the measles vaccine in Manassas VA, understanding the safety data can provide reassurance and confidence in your decision.
👉 Call today to schedule your child’s measles vaccine in Manassas.
Prevention remains far simpler than treatment.
CATEGORY
2/16/2026
POSTED
Measles is appearing in more communities across the U.S., and many parents are understandably concerned. While measles may feel like an illness from the past, it remains one of the most contagious viral infections affecting children today — and it often begins in a way that’s easy to miss.
How does measles start? How worried should I be? And when should I bring my child in?
This guide is designed to give parents clear, practical information so you can recognize symptoms early, understand how measles spreads, and feel confident about next steps if your child becomes ill.
What Is Measles and Why Is It So Contagious?
Measles is a viral illness that spreads through the air when an infected person coughs, sneezes, or breathes. Unlike many other childhood viruses, measles does not require close contact to spread.
The virus can remain in the air for up to two hours after an infected person leaves a room, meaning exposure can occur in classrooms, daycare centers, grocery stores, or medical offices without direct interaction.
What makes measles especially challenging is that children are contagious before parents realize it’s measles. By the time the classic rash appears, the virus may have already spread to others.
This is why early recognition and prevention play such an important role in protecting families and communities.
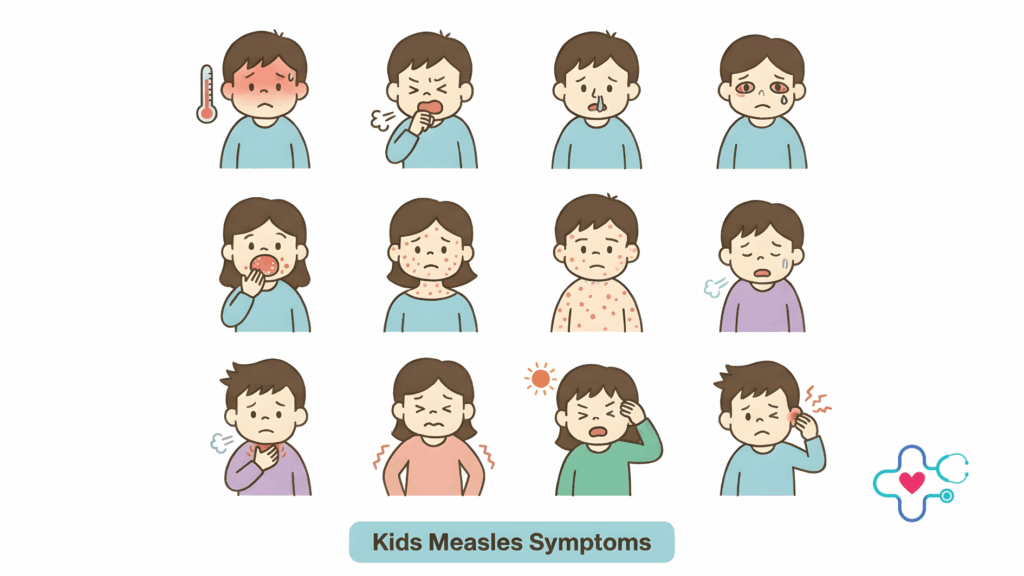
Early Measles Symptoms Parents Often Miss
Many parents associate measles with a rash — but the rash comes later.
In the early stage, measles often looks like a severe cold or flu. Symptoms may include:
- High fever, often rising quickly
- Cough
- Runny nose
- Red, watery, or irritated eyes
- Fatigue, irritability, or decreased appetite
Because these symptoms are common with many viral illnesses, measles can be difficult to identify at first. A key difference parents often notice is how sick their child looks and feels, especially when fever is high and persistent.
When the Rash Appears
The measles rash typically develops three to five days after fever begins. It usually:
- Starts on the face or hairline
- Spreads downward to the neck, trunk, arms, and legs
- Appears as flat red spots that may merge together
If your child develops fever followed by a spreading rash, or symptoms seem to worsen instead of improve, it’s important to contact a medical provider.
Why Measles Can Be Serious for Children
While many children recover from measles, it is not always a mild illness. Some children are at higher risk for complications, including:
- Infants under 12 months
- Children who are not fully vaccinated
- Children with asthma or chronic medical conditions
- Pregnant individuals and immunocompromised family members
Complications can include ear infections, dehydration, pneumonia, and in rare cases, serious neurologic issues. This is why prompt guidance and careful monitoring are important, even if symptoms seem manageable at first.
How Parents Can Protect Their Children From Measles
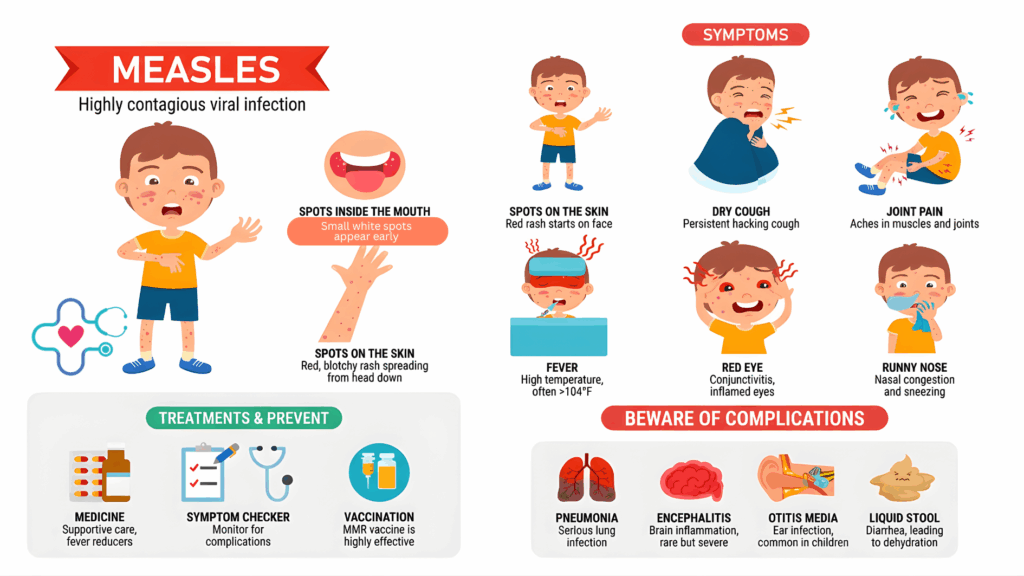
MMR Vaccination
The MMR (measles, mumps, rubella) vaccine is the most effective way to prevent measles. Two doses provide strong, long-lasting protection and significantly reduce the risk of severe illness and complications.
If you’re unsure whether your child is up to date on vaccinations or have questions about timing, a pediatric provider can help review your child’s immunization history and answer concerns.
Reducing Exposure
During times of increased measles activity:
- Avoid close contact with anyone who has fever and rash symptoms
- Be cautious in crowded indoor settings when possible
- Notify your healthcare provider if your child may have been exposed
Protecting High-Risk Family Members
If your household includes infants, pregnant individuals, or people with weakened immune systems, extra care is important. Keeping eligible family members vaccinated and limiting exposure to illness helps protect those most vulnerable.
When to Call Before Coming In
Because measles spreads so easily, calling ahead before visiting urgent care is essential.
Please contact a medical provider first if your child has:
- Fever along with a rash
- Known exposure to someone with measles
- Symptoms and is not fully vaccinated
Calling ahead allows our team to prepare appropriately and helps protect other children and families in our care.
Seek urgent or emergency care immediately if your child experiences:
- Trouble breathing or fast, labored breathing
- Extreme sleepiness, confusion, or difficulty staying awake
- Signs of dehydration such as very dry mouth, no tears, or minimal urination
- A very high fever that does not respond to medication
You never have to make these decisions alone. We are always here to help guide you.
For families seeking measles evaluation in Manassas, Night Watch Urgent Care provides walk-in pediatric care without long emergency room wait times.
Our pediatric-trained providers focus on early recognition, safe evaluation, and helping parents understand what to expect next.
CATEGORY
2/12/2026
POSTED
How to Know When Kitchen Injuries Need Professional Care
Your child is helping you cook.
The knife slips. Their finger’s bleeding.
You grab paper towels. Apply pressure. The bleeding slows down.
But when you look at it… it’s deep.
Do they need stitches? Or can you just bandage it?
Here’s how to know.
🔪 Cuts: The Stitches Decision Tree
Come to Night Watch if:
1. The Edges Gape Open
After you release pressure, do the edges pull apart? Can you see inside? Needs stitches.
2. It Won’t Stop Bleeding
After 10 minutes of continuous pressure, still bleeding steadily? Needs evaluation.
3. You Can See Fat, Muscle, or Bone
Needs stitches. Immediately.
4. It’s on Your Face or Hand
Facial cuts risk scarring. Hand cuts risk nerve/tendon damage. Both need professional evaluation.
5. It’s Over a Joint
Knuckles, knees, elbows. Movement pulls edges apart. Needs stitches or special closure.
6. Numbness or Weakness
Can’t feel your finger? Can’t move it normally? Possible nerve or tendon damage. Needs immediate care.
7. Caused by Something Dirty
Rusty knife? Dirty knife? Needs thorough cleaning and tetanus check.
8. It’s Been Hours
Cuts heal best when closed within 6-8 hours. After 12 hours, infection risk increases significantly.
🔥 Burns: First, Second, or Third Degree?
First-Degree Burns (Superficial)
What it looks like:
- Red, painful
- No blisters
- Like a bad sunburn
Treatment: Cool water, aloe, OTC pain relief. Usually okay to treat at home.
Second-Degree Burns (Partial Thickness)
What it looks like:
- Red, very painful
- BLISTERS
- May be wet/weeping
Come to Night Watch if:
- Larger than 3 inches
- On face, hands, feet, joints, or genitals
- Multiple large blisters
- Child or elderly patient
Third-Degree Burns (Full Thickness)
What it looks like:
- White, brown, or charred
- Leathery texture
- May NOT be painful (nerves destroyed)
Action: CALL 911 or go to ER immediately.
⏰ The Time Factor
For Cuts:
→ 0-6 hours: Ideal window for closure. Best healing, lowest infection risk.
→ 6-12 hours: Still can close, infection risk increasing.
→ 12+ hours: Often left open to heal, antibiotics likely needed.
For Burns:
Get evaluated same day. Burn severity isn’t always obvious initially. Infection can develop quickly.
What We Do at Night Watch
For Cuts:
- Thorough cleaning and irrigation
- Assess for nerve, tendon, or arterial damage
- Local anesthesia (numbing injection)
- Closure: Stitches, skin glue, or steri-strips depending on location/depth
- Wound care instructions and follow-up
For Burns:
- Assess burn depth and extent
- Clean and debride if needed
- Apply specialized burn dressings
- Pain management
- Antibiotics if infection risk high
- Refer to burn specialist if severe
Common Mistakes
For Cuts:
- Using super glue or duct tape (not sterile, risks infection)
- Assuming “it’ll be fine” (deep cuts need proper closure)
- Waiting days to seek care (infection sets in)
- Not checking tetanus status
For Burns:
- Putting ice directly on burn (damages tissue further)
- Applying butter, oil, or toothpaste (old wives’ tales, don’t work)
- Popping blisters (infection risk)
- Underestimating severity (“it’s just a little burn”)
🩹 Proper First Aid
For Cuts:
- Apply direct pressure with clean cloth (10 minutes minimum)
- Elevate above heart if possible
- Once bleeding stops, rinse with clean water
- Cover with clean bandage, then seek care if needed
For Burns:
- Remove from heat source immediately
- Cool under running water (not ice) for 10-20 minutes
- Remove jewelry/tight clothing from area
- Cover with clean, dry cloth
- Seek medical care if criteria met
The Bottom Line
→ When in doubt, come in. Better to have it checked.
→ Time matters. Don’t wait days.
→ Deep cuts need professional closure.
→ Second-degree burns need evaluation.
→ Face and hand injuries always get checked.
🔪 “Does this need stitches?” We can tell you for sure.
Get it checked before it gets infected.
CATEGORY
1/31/2026
POSTED
How to Tell—and What to Do About It
Your eyes are red. They’re itchy. There’s goop in the corners.
You Google: “red itchy eye” and everything says pink eye.
But is it really pink eye? And does it even need treatment?
Here’s what you need to know.
Not All Red Eyes Are Pink Eye
“Pink eye” (conjunctivitis) is inflammation of the conjunctiva – the clear membrane covering the white part of your eye.
But red eyes can also be:
- Dry eyes (from screen time, dry air, aging)
- Stye (infected eyelash follicle – bump on eyelid)
- Subconjunctival hemorrhage (broken blood vessel – bright red patch, not painful)
- Corneal abrasion (scratch on eye surface – painful)
- Foreign object (something in your eye)
How to tell if it’s actually pink eye:
- Discharge – Pink eye produces discharge. Dry eyes don’t.
- Crusting – Waking up with eyes sealed shut = pink eye
- Contagious spread – If others around you are getting it, likely pink eye
👀 The Three Types—How to Tell Them Apart
VIRAL Pink Eye
Symptoms:
- Watery, clear discharge
- Very itchy, very red
- Usually starts in one eye, spreads to other within 1-2 days
- Often accompanies cold symptoms
Caused by:
Adenovirus (same family as common cold)
Contagious?
EXTREMELY. Can spread for up to 2 weeks.
Treatment:
No antibiotics (it’s a virus). Supportive care—cool compresses, artificial tears. Runs its course in 7-14 days.
BACTERIAL Pink Eye
Symptoms:
- Thick, yellow or green discharge
- Eyes glued shut with crusty goop in morning
- More painful than viral
- Can affect one or both eyes
Caused by:
Bacteria (Staph, Strep, Haemophilus)
Contagious?
Yes, until treated with antibiotics.
Treatment:
Antibiotic eye drops. Usually clears in 3-5 days. Contagious until 24 hours after starting drops.
ALLERGIC Pink Eye
Symptoms:
- Both eyes affected at same time
- VERY itchy
- Watery discharge
- Other allergy symptoms (sneezing, runny nose)
Caused by:
Allergens (pollen, dust, pet dander, mold)
Contagious?
No.
Treatment:
Antihistamine eye drops, avoid allergen. Usually improves quickly.
When You Need to Come In
- Thick, colored discharge (likely bacterial = needs antibiotics)
- Eye pain or vision changes
- Sensitivity to light
- You wear contact lenses (higher infection risk)
- Symptoms not improving after 3-4 days
- You need a work note
- Newborn or infant with pink eye (always needs evaluation)
What We Do at Night Watch
- Examine eyes to determine type
- Rule out other causes (corneal abrasion, foreign object, etc.)
- Prescribe treatment (antibiotic drops for bacterial, supportive care for viral, antihistamines for allergic)
- Provide work/school notes
- Educate on preventing spread
🧼 Preventing Pink Eye
- Wash hands frequently – especially before touching eyes
- Don’t touch or rub eyes
- Don’t share towels, pillows, eye makeup, contact lens cases
- Replace eye makeup every 3 months, immediately after pink eye
- Clean contact lenses properly or use daily disposables
- Disinfect shared surfaces if someone in household has pink eye
❌ Common Mistakes
- Using old antibiotic drops from last time – they may be expired or contaminated
- Stopping antibiotics early – finish entire course
- Sharing drops between family members – spreads infection
- Wearing contacts during infection – can worsen and prolong infection
- Going to work/school before cleared – spreads to others
👁️ Red eyes? Goopy discharge? We can tell you what it is. Get the right diagnosis. Get the right treatment.
CATEGORY
1/20/2026
POSTED
Could Be Spraying Bacteria Into Their Face All Night
Let’s talk about your humidifier.
When’s the last time you cleaned it? Really cleaned it?
Not rinsed. Not “emptied the water.” Actually scrubbed, disinfected, and dried it?
If you’re thinking “…uh… never?” you’re not alone.
But here’s what’s happening inside that thing.
🦠 The Petri Dish in Your Kid’s Bedroom
A humidifier is basically a warm, wet, dark container.
Perfect environment for:
- Bacteria to multiply
- Mold to grow
- Biofilm to form (that slimy coating you can’t quite scrub off)
Within 24-48 hours of filling it with water, bacterial colonies start forming.
By day 3-4? Full-on bacterial party.
And every time you turn it on, it aerosolizes that bacteria-filled water and sprays it into the air your child breathes.
🔬 What Research Has Found
Studies analyzing home humidifiers found:
Legionella (Legionnaires’ Disease Bacteria)
Found in up to 32% of tested humidifiers. Causes severe pneumonia. Can be fatal in vulnerable populations.
Pseudomonas Aeruginosa
Common in hospital-acquired infections. Found frequently in home humidifiers. Causes respiratory infections, especially in people with compromised immune systems or chronic lung conditions.
Mold Spores (Aspergillus, Penicillium, Cladosporium)
Triggers asthma attacks, allergic reactions, and respiratory infections. Some molds produce mycotoxins (toxic compounds).
Endotoxins
Inflammatory compounds from bacterial cell walls. Cause fever, flu-like symptoms, and lung inflammation.
Mineral Deposits (“White Dust”)
From tap water minerals. Fine particles that settle on surfaces AND get inhaled. Can irritate lungs, especially in children with asthma.
“Humidifier Fever” & “Humidifier Lung”
These are real medical conditions:
Humidifier Fever (Endotoxin-Induced)
Symptoms:
- Fever and chills
- Body aches
- Headache
- Cough
Hypersensitivity Pneumonitis (“Humidifier Lung”)
Symptoms:
- Shortness of breath
- Persistent dry cough
- Chest tightness
- Fatigue
- Can cause permanent lung damage if exposure continues
The clue? Symptoms worsen at night (when humidifier runs) and improve during the day or away from home.
When to Come to Night Watch
- Persistent cough (especially worse at night)
- Wheezing or shortness of breath
- Chest tightness or pain
- Fever with respiratory symptoms
- Symptoms that improve away from home
- Recurring respiratory infections
We can evaluate for infections, provide breathing treatments, and help identify environmental triggers.
🧼 The REAL Cleaning Protocol
Most people don’t clean humidifiers nearly enough. Here’s what actually works:
EVERY DAY
- Empty ALL water (tank AND base)
- Rinse with clean water
- Wipe dry with clean towel
EVERY 3 DAYS
- Fill with undiluted white vinegar
- Let sit 30 minutes
- Scrub all surfaces with soft brush
- Rinse thoroughly until vinegar smell is gone
WEEKLY
- Disinfect with 3% hydrogen peroxide (fill tank, let sit 30 min)
- OR use diluted bleach (1 teaspoon per gallon water, 10 min soak)
- Rinse thoroughly multiple times (zero chemical residue)
ALWAYS
- Use ONLY distilled or demineralized water
- Replace filters per manufacturer schedule
- If you see/smell mold, throw it out and start fresh
Signs Your Humidifier Is Beyond Saving
- Black or green mold visible anywhere
- Persistent musty/moldy smell even after cleaning
- Thick biofilm that won’t scrub off
- Heavy mineral buildup that can’t be removed
- You literally can’t remember when you last cleaned it
If any of these apply? Throw it out. Buy a new one. Start fresh.
Better Alternatives
- Warm mist humidifiers: Boil water first, killing bacteria before releasing steam
- UV light models: Kill microorganisms before misting
- Low-tech options: Bowl of water on radiator, wet towels, houseplants
- Target 30-50% humidity: Higher than this promotes mold growth in your home
💧 You bought a humidifier to help. Don’t let it become the problem.
CATEGORY
1/16/2026
POSTED
Three Family Members at Urgent Care.
The new puppy has been home for one week.
Your daughter has scratches up and down her arms. Your son has a bite mark on his hand that’s looking puffy and red. And you? You’ve got a puncture wound from breaking up their “tug of war” that the puppy thought included your fingers.
Nobody told you this part of pet ownership.
Why Animal Bites Get Infected So Easily
Here’s the truth: animal mouths are bacteria factories.
Dogs, cats, puppies, kittens – their saliva contains dozens of types of bacteria. When they bite or lick an open wound, those bacteria get pushed deep into your tissue.
The result? Infection. And animal bite infections can get serious fast.
Infection rates by animal:
- Cat bites: 30-50% infection rate (high!)
- Dog bites: 10-20% infection rate
- Human bites: Actually the highest risk—but that’s another blog
Signs of Infection You Can’t Ignore
Come to Night Watch immediately if the bite or scratch shows:
- Redness spreading from the wound
- Red streaks going up the arm or leg
- Swelling, warmth, or increased pain
- Pus or drainage from the wound
- Fever
- Difficulty moving the affected area
- Swollen lymph nodes
These are signs your body is fighting an infection – and may be losing.
⏰ Time Matters
Here’s what people don’t realize: the sooner you get treatment, the better.
Within 8 hours of injury: Wound can be thoroughly cleaned, greatly reducing infection risk. May be able to close with stitches.
After 8 hours: Infection risk increases. May need to leave wound open. Antibiotics almost always needed.
After 24+ hours: If untreated, infection may have already started. Requires aggressive treatment.
Don’t wait. Come in the same day you’re bitten.
🐾 High-Risk Bites
Some bites are higher risk than others:
Hand Bites
Highest infection risk. Lots of small spaces for bacteria to hide. Close to tendons, joints, and bones. Always need medical evaluation.
Face Bites
Risk of scarring, nerve damage, and infection. Need immediate care.
Puncture Wounds
Look small on the surface but push bacteria deep into tissue. High infection risk. Often from cat bites.
Bites Through to Bone/Joint
Can cause bone or joint infection (osteomyelitis, septic arthritis). Serious. Need immediate treatment.
Treatment at Night Watch
We treat animal bites and scratches for all ages:
- Thorough wound irrigation (high-pressure cleaning to flush out bacteria)
- Examination for deep tissue damage
- X-rays if needed (to check for bone involvement)
- Stitches or wound closure (depending on type/location)
- Preventive antibiotics (especially for high-risk bites)
Preventing the Next Bite
- Supervise all pet interactions with children
- Start training immediately (puppy classes, bite inhibition)
- Don’t let pets mouth or play-bite people
- Keep kitten nails trimmed
- Redirect biting to appropriate toys
- Teach children to respect pet boundaries
New pets are adorable, infected animal bites are not. Get it treated before it gets serious.
CATEGORY
1/13/2026
POSTED
When Holiday Leftovers Turn Into a Family Health Crisis
You hosted the holiday gathering. The food was delicious. Everyone had seconds. Some people took leftovers home.
Now it’s three days later and your phone is blowing up:
“Hey, I’ve been throwing up since yesterday…”
“My kids are sick too…”
“Did anyone else get food poisoning from dinner?”
Uh oh.
When One Meal Takes Down Multiple People
Food poisoning doesn’t always happen because food was “old.” Sometimes it happens because:
- Food wasn’t cooked to the right temperature (undercooked poultry, stuffing)
- Food sat out too long (buffet style for 3+ hours)
- Cross-contamination happened (raw meat juice on veggies)
- Someone sick was handling food (norovirus spreads easily)
- Leftovers weren’t refrigerated quickly enough
If multiple people from the same meal get sick, it’s likely something at that dinner was contaminated.
Food Poisoning vs. Stomach Flu
Wait—how do you know it’s food poisoning and not just a stomach bug going around?
FOOD POISONING:
- Symptoms start suddenly (often within hours of eating)
- Everyone who ate the same thing gets sick
- Usually resolves in 24-48 hours
STOMACH FLU (NOROVIRUS):
- Spreads person-to-person over days
- Can be passed even without eating together
- Often includes fever and body aches
Either way? If symptoms are severe, come see us.
When to Seek Urgent Care
For Children:
- 🤢 Vomiting for more than 12 hours
- 💧 Can’t keep any liquids down
- 😴 Extreme lethargy or confusion
- 🚽 No wet diapers in 6+ hours
What We Can Do
At Night Watch, we treat food poisoning in children:
- IV fluids for rapid rehydration
- Anti-nausea and anti-diarrheal medications
- Stool testing to identify the bacteria
- Antibiotics (if bacterial infection is confirmed)
- Guidance on recovery and when to follow up
Prevention Tips for Next Time
- Use a meat thermometer: 165°F for poultry, 145°F for most other meats
- Don’t leave food out: Refrigerate within 2 hours (1 hour if it’s hot outside)
- Separate raw and cooked: Use different cutting boards and utensils
- Wash hands thoroughly: Before and after handling food
- When in doubt, throw it out: If it smells off or you can’t remember when you cooked it, toss it
CATEGORY
1/06/2026
POSTED
Flu season has arrived in Manassas, but with a few simple strategies, you can protect your family. Here’s what you need to know.
Get Your Flu Vaccine
Vaccination is the most effective way to prevent the flu. Everyone 6 months and older should get their annual flu shot, ideally in early fall before flu activity peaks. The vaccine takes about two weeks to become fully effective, so don’t wait.
Note: Children getting vaccinated for the first time may need two doses spaced four weeks apart.
Practice Good Hand Hygiene
Handwashing remains one of your best defenses against flu viruses. Encourage your kids to wash with soap and water for at least 20 seconds—singing a favorite song helps pass the time and makes it more enjoyable.
Key times to wash: before meals, after using the bathroom, after playing outside, and after coughing or sneezing.
Teach Proper Cough and Sneeze Etiquette
Show your children how to cough or sneeze into their elbow rather than their hands. This simple habit significantly reduces the spread of germs. Practice at home so it becomes automatic—many kids find it fun to “catch” their sneeze like a vampire in a cape.
Keep Sick Children Home
We know it’s challenging, but keeping feverish children home from school protects other children and gives your child time to recover. Kids should be fever-free for 24 hours without medication before returning to school or daycare.
Support Healthy Habits
A strong immune system makes a difference. Focus on the basics: adequate sleep, nutritious meals, regular physical activity, and plenty of water. These fundamentals help your child’s body fight off infections naturally.
Clean High-Touch Surfaces
During flu season, regularly wipe down frequently touched items like doorknobs, light switches, tablets, and toys. You don’t need to deep-clean constantly—just focus on these hotspots where germs tend to linger.
When to Contact Us
Most children recover from the flu at home with rest and fluids. However, call our office if your child has:
- Difficulty breathing or rapid breathing
- High fever over 104°F or fever lasting more than 3-4 days
- Signs of dehydration (no tears when crying, significantly decreased urination)
- Symptoms that improve then suddenly worsen
- Any concerns that something isn’t quite right
Trust your instincts—remember, you know your child best.
Stay Prepared, Not Worried
Flu season is manageable with the right approach. Get vaccinated, maintain good hygiene, keep sick kids home to rest, and support healthy habits. That’s really the foundation of flu prevention.
If your family does get sick despite your best efforts, remember that rest, comfort, and time usually do the trick. We’re here at Night Watch Manassas if you need us.
CATEGORY
11/17/2025
POSTED
Keep your kids safe this summer in Manassas! Night Watch Pediatric Urgent Care shares top tips to prevent dehydration, sunburn & heat exhaustion.
Summer fun in Manassas means trips to Signal Hill Park and local splash pads — but Virginia’s heat can lead to dehydration or heat exhaustion fast. Night Watch Pediatric Urgent Care wants local families to know how to stay safe and when to get help.
Tips:
√ Stay hydrated for outdoor fun at Baldwin Park and local pools
√ Reapply sunscreen every 2 hours
√ Use hats & sunglasses for extra sun protection
√ Check for ticks after hikes at Manassas National Battlefield
√ Know signs of heat exhaustion: dizziness, nausea, or headache
When to Visit Us: Come see us if your child shows signs of dehydration or severe sunburn.
We offer IV hydration for kids who need help bouncing back.
CATEGORY
7/10/2025