blog spot
THE
health hub
A collection of helpful articles & information to spread awareness through education from our staff to you
exacerbations — often triggered by recent weather changes.

Across Aldie (Stone Ridge), Manassas, and Winchester, more families are coming in with children experiencing coughing, wheezing, and breathing difficulties. In many cases, symptoms started mild but progressed quickly over a few days.
Seasonal transitions in Northern Virginia can make asthma harder to control — especially when temperature shifts, allergens, and viruses all overlap.
Why Weather Changes Trigger Asthma
Asthma affects the airways, making them more sensitive to environmental changes. When the weather shifts, the airways can become irritated and inflamed.
Cold air can cause the airways to tighten, while warmer conditions may increase exposure to allergens like pollen and mold. Rapid temperature changes — such as warm days followed by cool evenings — can also make it harder for children’s bodies to adjust.
At the same time, seasonal changes often bring more viral illnesses, which can further worsen asthma symptoms.
What Asthma Flare-Ups Can Look Like
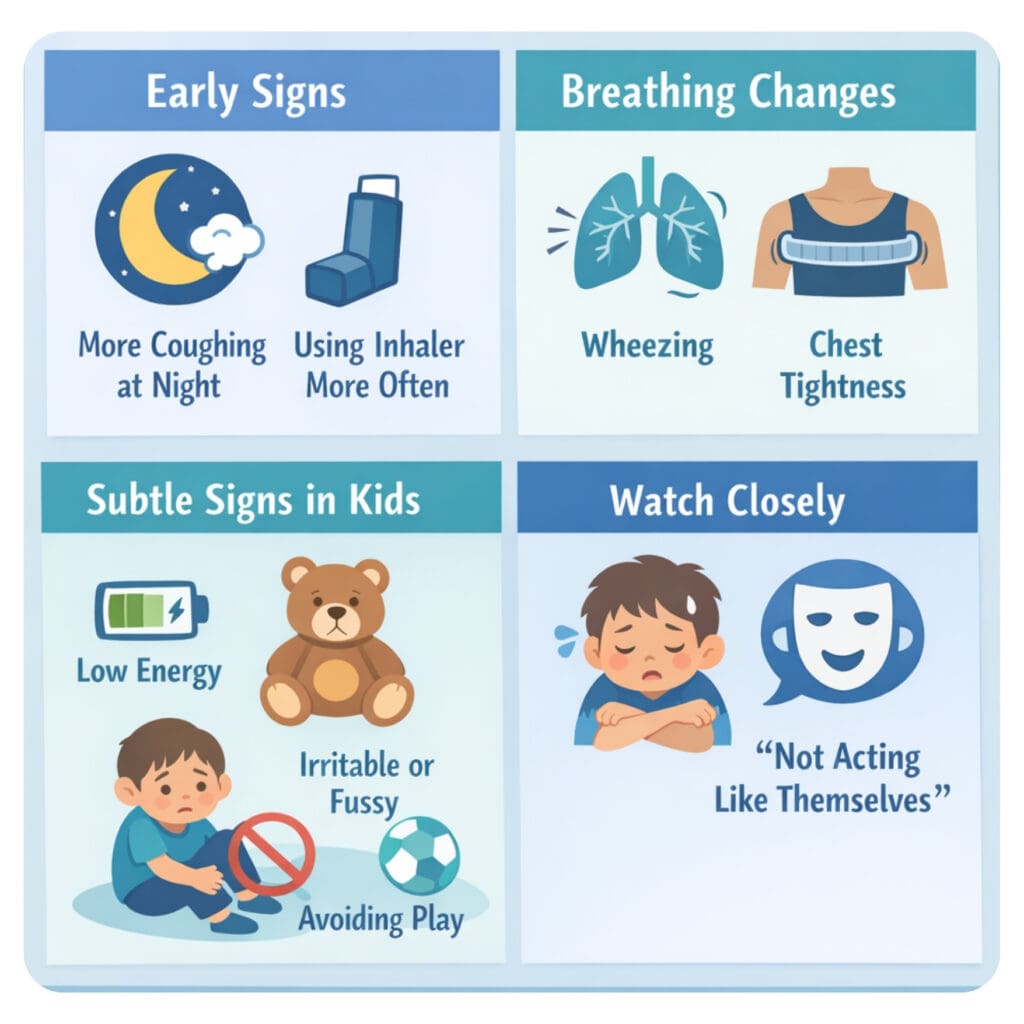
Asthma flare-ups don’t always start suddenly. Many begin with subtle symptoms that can be easy to overlook.
You may notice your child coughing more frequently, especially at night, or needing their inhaler more often than usual. Some children develop wheezing, which sounds like a whistling noise when breathing, while others may complain of chest tightness.
In younger children, symptoms may show up as low energy, irritability, or avoiding physical activity. Even small changes — like getting winded more easily or “not acting like themselves” — can be early signs that their breathing is affected.
When to Have Your Child Evaluated
If your child’s symptoms are not improving with home care or their usual medications, it may be time to have them evaluated.
At Night Watch Urgent Care, we regularly see children with asthma flare-ups who benefit from same-day care and early treatment. Addressing symptoms early can help prevent them from becoming more severe.
If your child is needing their inhaler more frequently, experiencing worsening cough, or having difficulty with normal activities, it’s best not to wait.
When Asthma Symptoms Become Urgent
Some symptoms require immediate medical attention.
If your child is breathing rapidly, using extra muscles to breathe (such as ribs pulling in or nostrils flaring), struggling to speak, or showing signs like bluish lips or unusual drowsiness, they should be taken to the emergency room right away.
These are signs of significant respiratory distress and should not be delayed.
Asthma Care at Night Watch Urgent Care
At Night Watch Urgent Care, we provide evaluation and treatment for asthma exacerbations and breathing concerns in children across Northern Virginia.
Our clinics offer:
- Same-day urgent care visits
- Breathing treatments, including nebulizer therapy
- On-site evaluation and monitoring
We’re open every day, including evenings and weekends, so families can access care when symptoms begin — not hours later.
Asthma flare-ups during weather changes are common — especially this time of year — but they can escalate quickly if not addressed early.
If your child’s symptoms are changing, worsening, or not improving, it’s always okay to have them checked.
CATEGORY
4/12/2026
POSTED
As the weather warms up in Northern Virginia, families are spending more time outdoors — at parks, trails, sports fields, and even in their own backyards. But with that increase in outdoor activity comes a higher risk of tick bites and Lyme disease.
According to a recent Loudoun County health update, tick season is highest from May through October, and our area continues to report some of the highest Lyme disease rates in Northern Virginia.
Understanding how to prevent tick bites — and recognizing early symptoms — can help protect your family during the months ahead.
What Is Lyme Disease?
Lyme disease is a bacterial infection spread through the bite of an infected blacklegged tick (also known as a deer tick).
These ticks are commonly found in wooded areas, tall grass, and brush, making everyday outdoor activities a potential source of exposure.
Lyme disease is the most common tick-borne illness in Loudoun County, but other tick-related illnesses can also occur, which is why awareness is important.
Signs and Symptoms of Lyme Disease
One of the challenges with Lyme disease is that symptoms don’t always appear right away — and many people don’t remember being bitten by a tick.
Early symptoms may include:
- Fever or chills
- Fatigue
- Headaches
- Muscle or joint pain
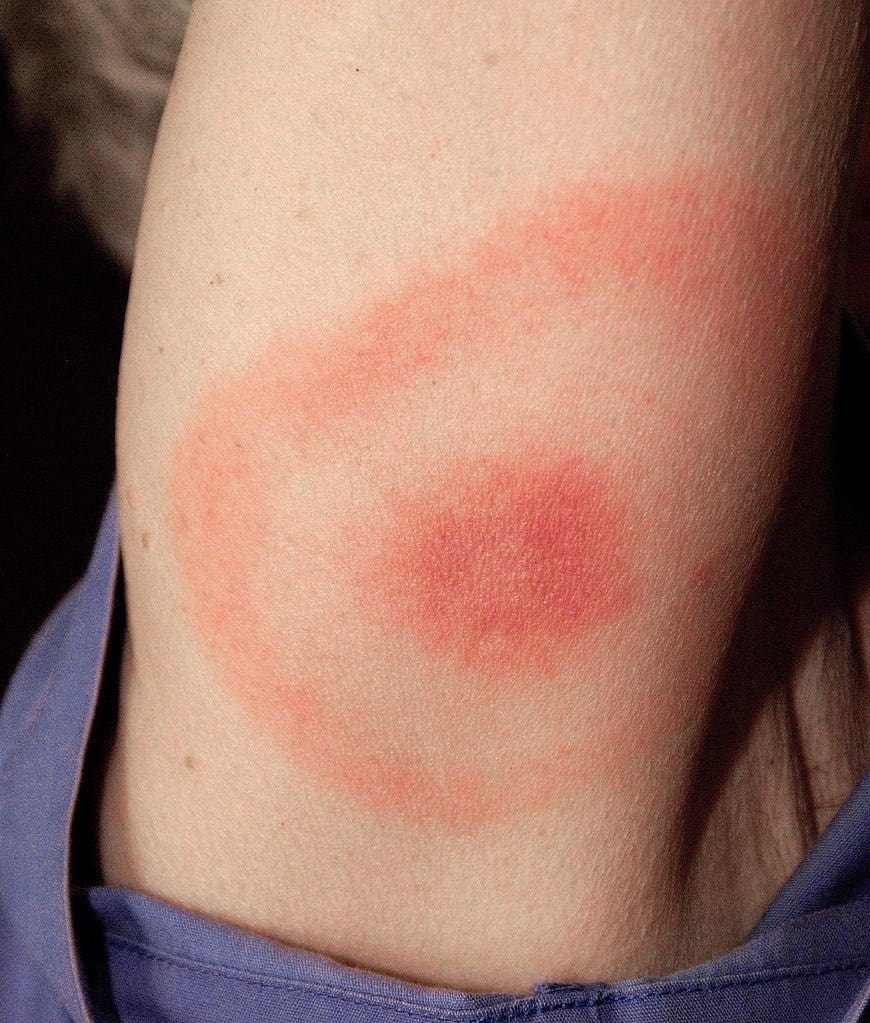
- A “bull’s-eye” rash (erythema migrans)
These symptoms can feel similar to a viral illness, which is why they’re sometimes overlooked.
If untreated, Lyme disease can affect the joints, heart, and nervous system, making early recognition and treatment especially important.
When Does Lyme Disease Spread?
Ticks can be active year-round, but risk is highest during warmer months.
In general, Lyme disease transmission usually requires a tick to be attached for at least 24 hours, although other tick-borne illnesses may spread more quickly.
Because tick bites are often painless and easy to miss, regular checks after outdoor activity are essential.
How to Prevent Tick Bites
Simple prevention steps can significantly reduce your risk of Lyme disease:
- Use insect repellent with 20% DEET or EPA-approved ingredients
- Wear long sleeves and long pants when outdoors
- Avoid tall grass and stay in the center of trails
- Choose light-colored clothing to spot ticks more easily
- Check your child’s skin, scalp, and clothing after outdoor activities
- Shower within two hours of coming indoors
- Place clothes in the dryer on high heat after outdoor exposure
- Remove ticks promptly with fine-tipped tweezers

These small habits can help protect both children and adults during peak tick season.
When Should You Get Checked?
You should consider medical evaluation if your child or family member has:
- A rash after outdoor exposure
- Flu-like symptoms during tick season
- Unexplained fatigue or joint pain
- A known or suspected tick bite
Even if symptoms seem mild, early evaluation can help guide next steps and prevent complications.
Lyme Disease Care in Loudoun County and Northern Virginia
At Night Watch Urgent Care, we evaluate tick bites, rashes, and symptoms of Lyme disease with same-day care across Northern Virginia.
Our providers understand that early symptoms can be subtle, and we’re here to help you determine whether further evaluation or treatment is needed.
We’re open evenings and weekends, so you don’t have to wait to get your child checked.
CATEGORY
4/06/2026
POSTED
Respiratory symptoms in children are becoming more common across the United States, especially during seasonal transitions. Many healthcare providers are reporting an increase in cough, wheezing, and asthma flare-ups in children, often triggered by a mix of viruses, allergies, and weather changes.
We’re seeing the same pattern locally at Night Watch Urgent Care in Stone Ridge (Aldie), Manassas, and Winchester, where more families are coming in with concerns about their child’s breathing.
For many children, symptoms begin mild — a simple cough or slight fatigue — but can progress quickly if not monitored closely.

Common Breathing Symptoms in Kids
Breathing problems in children don’t always look severe at first, which can make it difficult for parents to know when to be concerned.
A frequent or worsening cough, especially at night, is often one of the earliest signs. Some children may start needing their inhaler more often than usual, while others develop a wheezing or whistling sound when breathing, which can indicate narrowed airways.
In other cases, children may complain of chest tightness or appear more tired than usual. Subtle changes — like avoiding play, getting winded easily, or simply “not acting like themselves” — can be early indicators that their breathing is affected.
Recognizing these signs early can help prevent symptoms from worsening.

When to Bring Your Child to Urgent Care
If your child’s symptoms are not improving with home care or their usual medications, it may be time to have them evaluated.
At Night Watch Urgent Care, we regularly treat children with asthma flare-ups, persistent cough, and breathing difficulties who benefit from same-day care. Early evaluation allows providers to assess your child’s breathing, adjust treatment if needed, and help prevent symptoms from escalating.
Seeking care sooner rather than later can reduce the likelihood of needing emergency treatment.
When Breathing Symptoms Become Urgent
Some symptoms require immediate medical attention and should not be delayed.
If your child is breathing rapidly, struggling to catch their breath, using extra muscles to breathe (such as ribs pulling in or nostrils flaring), or having difficulty speaking, they should be taken to the emergency room right away.
Other warning signs include bluish lips or face, extreme fatigue, or unusual drowsiness. These may indicate serious respiratory distress and require urgent care.
Pediatric Urgent Care for Breathing Issues in Northern Virginia
At Night Watch Urgent Care, we provide evaluation and treatment for asthma flare-ups, wheezing, and respiratory symptoms in children across Northern Virginia.
Our clinics offer:
- Same-day urgent care visits
- Breathing treatments, including nebulizer therapy
- On-site evaluation and monitoring
We’re open every day, including evenings and weekends, so families can access care when symptoms start — not hours later.
CATEGORY
3/30/2026
POSTED
6 Things Night Watch Urgent Care Does Differently
When your child gets sick or injured, one of the hardest decisions parents face is where to go. Should you wait for your pediatrician? Head to the emergency room? Or look for an urgent care that actually understands pediatric needs?
At Night Watch Urgent Care, we’ve built our clinics around what families truly need: convenience, clarity, and care that fits real life.
Here are six ways we do things differently.
1. Pediatric Urgent Care Designed for Real Life
We are not just an urgent care clinic — we are a pediatric-focused environment designed to make children feel comfortable and supported.
From common illnesses like fevers and coughs to injuries that happen during play or sports, our approach centers on both medical care and the overall experience for families.
2. Open Late and on Weekends
Illness doesn’t follow office hours, and neither do we.
⏰ Hours:
Monday–Friday: 10 AM – 10 PM
Saturday–Sunday: 10 AM – 7 PM
Whether symptoms start after school or worsen at night, families have access to care when they actually need it.
3. We Treat More Than You Might Expect
Many parents are surprised by the range of conditions we manage.
We regularly treat:
• Flu symptoms and respiratory illnesses
• Ear infections and sore throats
• Minor fractures, sprains, and sports injuries
• Cuts that require stitches
• Rashes and allergic reactions
• Dehydration and stomach illnesses
This means fewer referrals and fewer stops for care.
4. On-Site X-Rays and Testing
One of the biggest advantages of visiting Night Watch Urgent Care is access to immediate diagnostics.
With on-site X-rays and testing, we can:
• Confirm fractures
• Evaluate injuries
• Diagnose infections
• Provide same-visit treatment plans
Families don’t have to wait days for answers or travel to multiple locations.
5. Helping Families Avoid Unnecessary ER Visits
Emergency rooms are essential for serious, life-threatening conditions — but many situations fall into a gray area.
When it’s urgent but not an emergency, urgent care is often the right choice.
At Night Watch, we provide timely evaluation and treatment so families can avoid long ER wait times and higher costs when appropriate.
6. Care for Both Kids and Adults at Stone Ridge
📍 Stone Ridge Location
In addition to pediatric care, this location also treats adults.
This makes it easier for families to receive care together, especially when multiple members are feeling unwell or need evaluation at the same time.

Convenient Care Across Northern Virginia
Night Watch Urgent Care serves families across:
• Manassas
• Winchester
• Aldie / Stone Ridge
With extended hours, comprehensive services, and a family-centered approach, we are here when care can’t wait.
When to Visit Night Watch Urgent Care
If your child is sick, injured, or something simply doesn’t feel right, it’s always okay to seek care.
Having access to a trusted urgent care can make these moments less stressful and more manageable.
We are open late and available on weekends to support your family’s needs.
Care should be accessible, efficient, and built around real life — and that’s exactly what we aim to provide.
CATEGORY
3/23/2026
POSTED
the past seven years, Night Watch Urgent Care has been proud to serve families across Northern Virginia by providing trusted pediatric urgent care when children need it most.
What began as a mission to make healthcare more accessible for families has grown into a reliable resource for parents looking for evening and weekend pediatric care outside traditional office hours.
Over the years, our clinics have helped thousands of families navigate everything from late-night fevers and sudden illnesses to minor injuries and unexpected health concerns.

Supporting Families When It Matters Most
Children rarely get sick at convenient times. Many parents find themselves searching for urgent care for kids near them late at night or on weekends when their pediatrician’s office is closed.
That is exactly why Night Watch Urgent Care exists.
Our team provides accessible pediatric urgent care services, helping families receive timely medical attention without the long wait times often associated with emergency rooms.
Common reasons families visit our clinics include:
• Fevers and viral illnesses
• Ear infections
• Cough, wheezing, and breathing concerns
• Minor injuries and fractures
• Rashes and allergic reactions
• Vomiting and dehydration
• Concussions and head injuries
Every visit is an opportunity to provide reassurance, answers, and compassionate care for both children and parents.
Pediatric Care That Focuses on Families
At Night Watch Urgent Care, pediatric care goes beyond treating symptoms. We focus on creating an environment where children feel comfortable and parents feel supported.
Our providers understand that when a child is sick, families need more than just medical treatment. They need guidance, clear communication, and confidence that they are making the right decisions for their child’s health.
For the past seven years, families have trusted our team to provide that care, and we are deeply grateful for the opportunity to serve our community.
Thank You for Trusting Us
Reaching this seven-year milestone would not have been possible without the families who have chosen Night Watch Urgent Care for their children’s healthcare needs.
We are incredibly thankful to the parents, caregivers, and children who have walked through our doors, called us for guidance, or trusted us during difficult moments.
Serving this community is an honor, and we look forward to continuing to support the health and well-being of families for many years to come.
Pediatric Urgent Care When You Need It
Night Watch Urgent Care provides convenient pediatric urgent care with evening and weekend availability, making it easier for families to get care when traditional offices are closed.
Walk-ins are welcome.
Stone Ridge (Aldie, VA)
42010 Village Center Plaza, Ste 100
(703) 775-4999
Winchester, VA
2118 Pleasant Valley Rd
(540) 545-9999
Manassas, VA
11700 Sudley Manor Dr
(703) 589-9695
If you are searching for pediatric urgent care near you, our team is here to help.
Share Your Experience
If Night Watch Urgent Care has cared for your family over the years, we would love to hear your story. Your feedback helps us continue improving and supporting families across our community.
Thank you for being part of our journey.
CATEGORY
3/10/2026
POSTED
Recent public health reports confirm that measles cases are increasing again in parts of the United States. While outbreaks may not be widespread in every region, the virus’s ability to spread rapidly makes vaccination status an important topic for families in Manassas.
The most effective protection remains full immunization with the MMR vaccine.

Understanding the Risk
Measles spreads through the air and can infect individuals who were never in direct contact with a sick person. Because symptoms initially resemble a routine viral illness, measles can circulate for days before being identified.
Early symptoms often include high fever, cough, runny nose, and red eyes. The rash appears later. By that point, a child may already have exposed others.
Although many children recover, complications can include pneumonia, dehydration, ear infections, and in rare cases, brain inflammation. Hospitalization is not uncommon in outbreak settings.
These risks are significantly reduced in vaccinated children.
It is common for parents to have questions about vaccine safety. The MMR vaccine has been extensively studied worldwide and continues to be monitored for safety. Side effects are generally mild and temporary, such as soreness at the injection site or a low-grade fever.
If you have concerns, discussing them with a pediatric provider allows for informed decision-making based on evidence rather than misinformation.
If your child is due for an MMR vaccine in Manassas, now is the time to confirm protection.
How Effective Is the MMR Vaccine?
The MMR vaccine protects against measles, mumps, and rubella. For measles specifically:
• One dose is approximately 93 percent effective
• Two doses are approximately 97 percent effective
That level of protection is considered extremely strong in preventive medicine. For most children who receive both recommended doses, immunity is long-lasting.
The standard schedule recommended by the CDC is:
• First dose between 12 and 15 months
• Second dose between 4 and 6 years
If your child has received both doses, they are highly protected. If you are unsure, this is the time to review records.
Is the Measles (MMR) Vaccine Safe for Children?
Safety is often the first concern for families in Manassas considering immunizations. The MMR vaccine is one of the most extensively studied vaccines in pediatric medicine.
Before approval, vaccines must pass through:
• Pre-clinical laboratory testing
• Phase 1, 2, and 3 clinical trials
• FDA review
• Ongoing post-licensure monitoring
Even after decades of use, safety monitoring continues through national reporting systems.
The vast majority of children tolerate the MMR vaccine without issue. When side effects occur, they are generally mild and short-lived, including:
• Temporary soreness at the injection site
• Low-grade fever
• Mild rash
Severe allergic reactions are extremely rare.
Extensive research has shown no association between the MMR vaccine and autism. Multiple international studies have confirmed its safety profile.
From a medical standpoint, the risk of measles infection — including complications like pneumonia or encephalitis — far outweighs the risk of vaccine side effects.
For families searching for the measles vaccine in Manassas VA, understanding the safety data can provide reassurance and confidence in your decision.
👉 Call today to schedule your child’s measles vaccine in Manassas.
Prevention remains far simpler than treatment.
CATEGORY
2/16/2026
POSTED
Measles is appearing in more communities across the U.S., and many parents are understandably concerned. While measles may feel like an illness from the past, it remains one of the most contagious viral infections affecting children today — and it often begins in a way that’s easy to miss.
How does measles start? How worried should I be? And when should I bring my child in?
This guide is designed to give parents clear, practical information so you can recognize symptoms early, understand how measles spreads, and feel confident about next steps if your child becomes ill.
What Is Measles and Why Is It So Contagious?
Measles is a viral illness that spreads through the air when an infected person coughs, sneezes, or breathes. Unlike many other childhood viruses, measles does not require close contact to spread.
The virus can remain in the air for up to two hours after an infected person leaves a room, meaning exposure can occur in classrooms, daycare centers, grocery stores, or medical offices without direct interaction.
What makes measles especially challenging is that children are contagious before parents realize it’s measles. By the time the classic rash appears, the virus may have already spread to others.
This is why early recognition and prevention play such an important role in protecting families and communities.
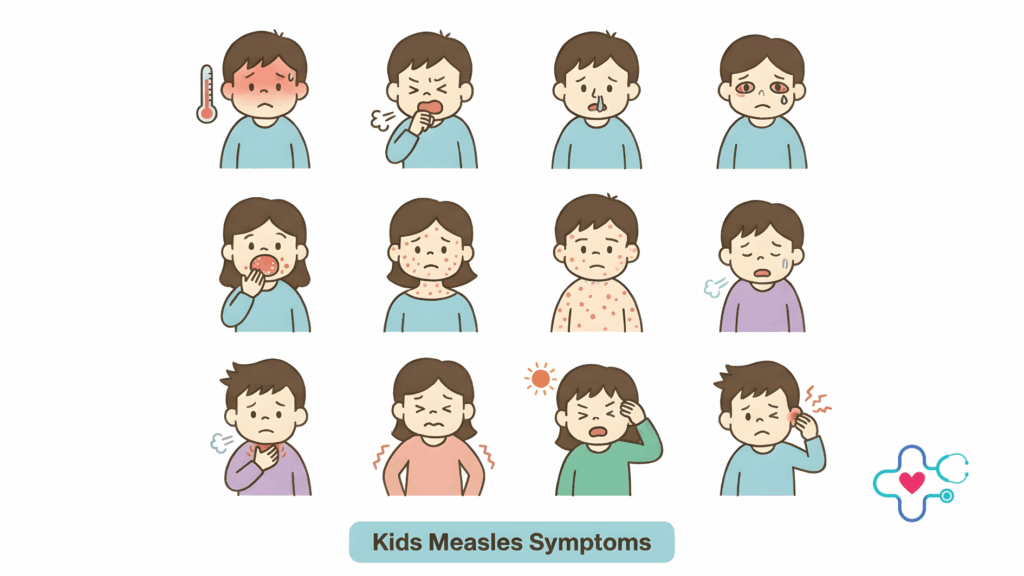
Early Measles Symptoms Parents Often Miss
Many parents associate measles with a rash — but the rash comes later.
In the early stage, measles often looks like a severe cold or flu. Symptoms may include:
- High fever, often rising quickly
- Cough
- Runny nose
- Red, watery, or irritated eyes
- Fatigue, irritability, or decreased appetite
Because these symptoms are common with many viral illnesses, measles can be difficult to identify at first. A key difference parents often notice is how sick their child looks and feels, especially when fever is high and persistent.
When the Rash Appears
The measles rash typically develops three to five days after fever begins. It usually:
- Starts on the face or hairline
- Spreads downward to the neck, trunk, arms, and legs
- Appears as flat red spots that may merge together
If your child develops fever followed by a spreading rash, or symptoms seem to worsen instead of improve, it’s important to contact a medical provider.
Why Measles Can Be Serious for Children
While many children recover from measles, it is not always a mild illness. Some children are at higher risk for complications, including:
- Infants under 12 months
- Children who are not fully vaccinated
- Children with asthma or chronic medical conditions
- Pregnant individuals and immunocompromised family members
Complications can include ear infections, dehydration, pneumonia, and in rare cases, serious neurologic issues. This is why prompt guidance and careful monitoring are important, even if symptoms seem manageable at first.
How Parents Can Protect Their Children From Measles
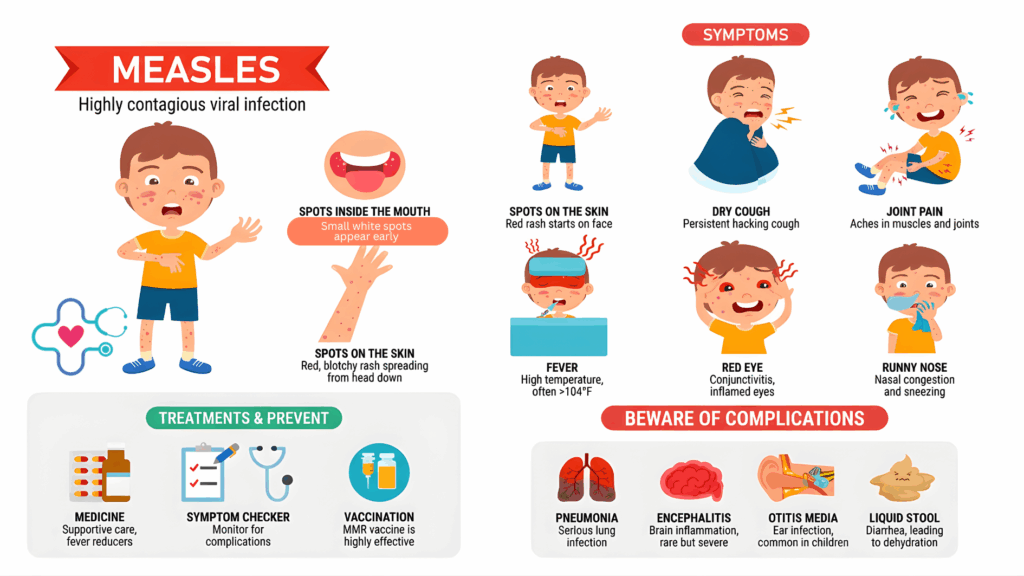
MMR Vaccination
The MMR (measles, mumps, rubella) vaccine is the most effective way to prevent measles. Two doses provide strong, long-lasting protection and significantly reduce the risk of severe illness and complications.
If you’re unsure whether your child is up to date on vaccinations or have questions about timing, a pediatric provider can help review your child’s immunization history and answer concerns.
Reducing Exposure
During times of increased measles activity:
- Avoid close contact with anyone who has fever and rash symptoms
- Be cautious in crowded indoor settings when possible
- Notify your healthcare provider if your child may have been exposed
Protecting High-Risk Family Members
If your household includes infants, pregnant individuals, or people with weakened immune systems, extra care is important. Keeping eligible family members vaccinated and limiting exposure to illness helps protect those most vulnerable.
When to Call Before Coming In
Because measles spreads so easily, calling ahead before visiting urgent care is essential.
Please contact a medical provider first if your child has:
- Fever along with a rash
- Known exposure to someone with measles
- Symptoms and is not fully vaccinated
Calling ahead allows our team to prepare appropriately and helps protect other children and families in our care.
Seek urgent or emergency care immediately if your child experiences:
- Trouble breathing or fast, labored breathing
- Extreme sleepiness, confusion, or difficulty staying awake
- Signs of dehydration such as very dry mouth, no tears, or minimal urination
- A very high fever that does not respond to medication
You never have to make these decisions alone. We are always here to help guide you.
For families seeking measles evaluation in Manassas, Night Watch Urgent Care provides walk-in pediatric care without long emergency room wait times.
Our pediatric-trained providers focus on early recognition, safe evaluation, and helping parents understand what to expect next.
CATEGORY
2/12/2026
POSTED
How to Know When Kitchen Injuries Need Professional Care
Your child is helping you cook.
The knife slips. Their finger’s bleeding.
You grab paper towels. Apply pressure. The bleeding slows down.
But when you look at it… it’s deep.
Do they need stitches? Or can you just bandage it?
Here’s how to know.
🔪 Cuts: The Stitches Decision Tree
Come to Night Watch if:
1. The Edges Gape Open
After you release pressure, do the edges pull apart? Can you see inside? Needs stitches.
2. It Won’t Stop Bleeding
After 10 minutes of continuous pressure, still bleeding steadily? Needs evaluation.
3. You Can See Fat, Muscle, or Bone
Needs stitches. Immediately.
4. It’s on Your Face or Hand
Facial cuts risk scarring. Hand cuts risk nerve/tendon damage. Both need professional evaluation.
5. It’s Over a Joint
Knuckles, knees, elbows. Movement pulls edges apart. Needs stitches or special closure.
6. Numbness or Weakness
Can’t feel your finger? Can’t move it normally? Possible nerve or tendon damage. Needs immediate care.
7. Caused by Something Dirty
Rusty knife? Dirty knife? Needs thorough cleaning and tetanus check.
8. It’s Been Hours
Cuts heal best when closed within 6-8 hours. After 12 hours, infection risk increases significantly.
🔥 Burns: First, Second, or Third Degree?
First-Degree Burns (Superficial)
What it looks like:
- Red, painful
- No blisters
- Like a bad sunburn
Treatment: Cool water, aloe, OTC pain relief. Usually okay to treat at home.
Second-Degree Burns (Partial Thickness)
What it looks like:
- Red, very painful
- BLISTERS
- May be wet/weeping
Come to Night Watch if:
- Larger than 3 inches
- On face, hands, feet, joints, or genitals
- Multiple large blisters
- Child or elderly patient
Third-Degree Burns (Full Thickness)
What it looks like:
- White, brown, or charred
- Leathery texture
- May NOT be painful (nerves destroyed)
Action: CALL 911 or go to ER immediately.
⏰ The Time Factor
For Cuts:
→ 0-6 hours: Ideal window for closure. Best healing, lowest infection risk.
→ 6-12 hours: Still can close, infection risk increasing.
→ 12+ hours: Often left open to heal, antibiotics likely needed.
For Burns:
Get evaluated same day. Burn severity isn’t always obvious initially. Infection can develop quickly.
What We Do at Night Watch
For Cuts:
- Thorough cleaning and irrigation
- Assess for nerve, tendon, or arterial damage
- Local anesthesia (numbing injection)
- Closure: Stitches, skin glue, or steri-strips depending on location/depth
- Wound care instructions and follow-up
For Burns:
- Assess burn depth and extent
- Clean and debride if needed
- Apply specialized burn dressings
- Pain management
- Antibiotics if infection risk high
- Refer to burn specialist if severe
Common Mistakes
For Cuts:
- Using super glue or duct tape (not sterile, risks infection)
- Assuming “it’ll be fine” (deep cuts need proper closure)
- Waiting days to seek care (infection sets in)
- Not checking tetanus status
For Burns:
- Putting ice directly on burn (damages tissue further)
- Applying butter, oil, or toothpaste (old wives’ tales, don’t work)
- Popping blisters (infection risk)
- Underestimating severity (“it’s just a little burn”)
🩹 Proper First Aid
For Cuts:
- Apply direct pressure with clean cloth (10 minutes minimum)
- Elevate above heart if possible
- Once bleeding stops, rinse with clean water
- Cover with clean bandage, then seek care if needed
For Burns:
- Remove from heat source immediately
- Cool under running water (not ice) for 10-20 minutes
- Remove jewelry/tight clothing from area
- Cover with clean, dry cloth
- Seek medical care if criteria met
The Bottom Line
→ When in doubt, come in. Better to have it checked.
→ Time matters. Don’t wait days.
→ Deep cuts need professional closure.
→ Second-degree burns need evaluation.
→ Face and hand injuries always get checked.
🔪 “Does this need stitches?” We can tell you for sure.
Get it checked before it gets infected.
CATEGORY
1/31/2026
POSTED
How to Tell the Difference (And When to Worry)
You’ve been staring at screens all day.
Now your head hurts.
Is it just digital eye strain? Or something more serious?
Let’s break it down.
📱 Digital Eye Strain Headaches
What It Feels Like:
- Dull ache across forehead or temples
- Pressure behind eyes
- Starts gradually after screen use
- Gets worse the longer you’re on screens
- Improves when you take breaks
Other Symptoms:
- Dry, irritated eyes
- Blurry vision
- Neck and shoulder tension
- Light sensitivity
Treatment:
Take screen breaks, use 20-20-20 rule, artificial tears, better ergonomics. Usually resolves on its own.
Migraine Headaches
What It Feels Like:
- Intense, throbbing pain (often one-sided)
- Can be triggered by screens but feels different
- Moderate to severe intensity
- Lasts 4 – 72 hours if untreated
- Gets worse with physical activity
Other Symptoms:
- Nausea or vomiting
- Extreme light and sound sensitivity
- Visual disturbances (aura) before headache
- Need to lie down in dark, quiet room
Treatment:
Migraine medications, dark room, rest. May need prescription treatment if frequent.
💢 Tension Headaches
What It Feels Like:
- Band-like tightness around head
- Both sides of head affected
- Mild to moderate pain
- Related to stress, poor posture, or muscle tension
Screen-Related Cause:
Hunching over devices → neck strain → tension headache. Very common with prolonged screen use.
When It’s NOT Just Screen Time
Come to Night Watch immediately if:
- Worst headache of your life (“thunderclap headache”)
- Headache with fever, stiff neck, or confusion
- Vision loss or double vision
- Sudden onset after head injury
- Weakness, numbness, or difficulty speaking
- Headache that wakes you from sleep
- New headache pattern in someone over 50
These could indicate serious conditions requiring immediate evaluation.
Vision Problems vs. Eye Strain
Digital Eye Strain:
- Temporary blurry vision that clears with breaks
- Improves when not using screens
- Both eyes affected similarly
Actual Vision Problems:
- Persistent blurry vision
- Double vision
- Halos around lights
- One eye affected more than other
- Sudden vision changes
If vision problems persist after screen breaks, you need an eye exam.
What We Do at Night Watch
When you come in with headaches or vision concerns:
- Detailed history (headache pattern, triggers, associated symptoms)
- Physical and neurological exam
- Visual screening
- Rule out serious causes (infections, neurological issues)
- Provide treatment (pain relief, migraine meds if appropriate)
- Refer to specialists (ophthalmology, neurology) if needed
Prevention Strategies
For Screen-Related Headaches:
- 20-20-20 rule (every 20 min, look 20 feet away for 20 sec)
- Proper ergonomics (screen position, chair height, lighting)
- Blue light filters (especially evening)
- Adequate breaks (get up, move around)
- Adjust screen brightness (match room lighting)
For Migraines:
- Identify and avoid triggers
- Consistent sleep schedule
- Hydration
- Stress management
- Consider preventive medications if frequent
The Bottom Line
→ Most screen-related headaches are eye strain or tension headaches
→ They improve with breaks and better habits
→ Migraines are more severe and come with other symptoms
→ Sudden, severe, or unusual headaches need evaluation
→ When in doubt, get it checked
🤕 Screen headache or something more serious? We can help you figure it out.
CATEGORY
1/29/2026
POSTED
When Should You Actually Test Their Immune System?
Your child has been sick seven times since September.
You’re keeping a tally. You’ve used all your sick days. You’re starting to wonder if something is actually wrong.
Should you ask for immune testing?
Let’s walk through this.
What is “Immune Deficiency”?
Primary immunodeficiency disorders (PIDDs) are genetic conditions where the immune system doesn’t work properly.
How common are they?
Rare. About 1 in 1,200 people. Most are diagnosed in childhood.
Translation: If your child gets lots of colds, it’s probably not an immune deficiency. But if they meet certain criteria, testing might be warranted.
The “10 Warning Signs”
The Jeffrey Modell Foundation (experts in immune deficiency) lists 10 warning signs:
- 1. 4+ new ear infections in one year
- 2. 2+ serious sinus infections in one year
- 3. 2+ months on antibiotics with little effect
- 4. 2+ pneumonias in one year
- 5. Failure to gain weight or grow normally
- 6. Recurrent deep skin or organ abscesses
- 7. Persistent thrush or fungal infections
- 8. Need for IV antibiotics to clear infections
- 9. 2+ deep-seated infections (meningitis, sepsis, bone infection)
- 10. Family history of primary immunodeficiency
Notice what’s NOT on this list:
“Lots of colds.”
Normal vs. Concerning
✅ PROBABLY NORMAL
- 6 -12 colds per year
- 2-3 stomach bugs per year
- Occasional ear infections that respond to antibiotics
- Pink eye once or twice
- Hand-foot-mouth disease, croup, etc.
⚠️ POTENTIALLY CONCERNING
- Multiple pneumonias
- Recurrent sinus infections requiring antibiotics
- Ear infections that don’t respond to treatment
- Deep infections (blood, bone, organs)
- Chronic diarrhea + poor growth
- Unusual infections (fungal, atypical bacteria)
It’s the TYPE and SEVERITY of infections that matter, not just the frequency.
What Immune Testing Involves
If testing is warranted, we typically start with:
Complete Blood Count (CBC)
Checks overall white blood cell counts and types
Immunoglobulin Levels
Measures antibody levels (IgG, IgA, IgM, IgE)
Vaccine Response Testing
Checks if body made antibodies to vaccines they’ve received
More specialized testing (genetic testing, T-cell function, etc.) is done by immunology specialists if initial tests are concerning.
How We Help at Night Watch
When you bring your frequently-sick child to us:
- Review their illness history
- Diagnose current illness (strep, flu, ear infection, etc.)
- Evaluate patterns (are these serious infections or common colds?)
- Order initial testing if warranted (CBC, immunoglobulins)
- Refer to immunology specialists if testing suggests immune deficiency
- Reassure you when it’s normal childhood illness
📝 What to Track
Keep a log if you’re concerned:
- Date and type of each illness
- Whether antibiotics were needed
- How well they responded to treatment
- Any hospitalizations or ER visits
- Growth patterns (height/weight)
Bring this to your visit. It helps us see the big picture.
The Bottom Line
→ Most kids who get sick frequently have normal immune systems
→ 6 -12 illnesses per year is textbook normal for young children
→ It’s the severity and type of infections that matter, not just frequency
→ True immune deficiency is rare
→ If you meet warning criteria, testing is appropriate
🤧 Worried about recurrent illness? We can evaluate.
Most of the time, it’s normal. But we’ll help you know for sure.
CATEGORY
1/22/2026