blog spot
THE
health hub
A collection of helpful articles & information to spread awareness through education from our staff to you
May is Urgent Care Awareness Month, a time to recognize the critical role urgent care plays in keeping communities healthy, and to help families understand when and how to use it.
For families across Northern Virginia, Night Watch Urgent Care has been that resource since 2019. Not a corporate chain. Not a crowded ER. Just a locally owned team of experienced providers who show up every day, including evenings and weekends, for the moments that cannot wait.
This month we want to share why so many families in Loudoun County, Manassas, and Winchester have made Night Watch their first call when something comes up.
What Urgent Care Awareness Month Is All About
Urgent Care Awareness Month was created to educate communities about the important role urgent care centers play in the healthcare system.
Urgent care fills the gap between a primary care office and an emergency room. It is designed for conditions that need same-day attention but are not life threatening. Conditions that cannot wait for a Monday morning appointment, but also do not need a four-hour ER visit.
The goal of Urgent Care Awareness Month is simple: help people make better, faster healthcare decisions so they get the right care in the right place at the right time.
And in Northern Virginia, Night Watch is that place for thousands of families every year.
Why Northern Virginia Families Choose Night Watch
Locally Owned and Operated
Night Watch was not built by a corporation. It was built by a board-certified pediatrician and local entrepreneur who saw a real need in the community and decided to do something about it.
That matters. When you walk through our doors, you are not a number in a system. You are a neighbor. Our providers know their patients, treat families like their own, and have built a practice grounded in genuine care.
No corporate phone trees. No impersonal systems. Just a team that is invested in the health of this community.
Open When Your Pediatrician Is Not
Kids get sick at 8pm on a Friday. Fevers spike at midnight. Injuries happen on Sunday afternoons.
Night Watch is open Monday through Friday until 10pm and every weekend from 10am to 7pm. That means when your child comes home from school feeling off, or your toddler wakes up at 9pm with ear pain, you have somewhere to go tonight.
You do not have to wait. You do not have to guess. You can walk in.
Same Urgent Care for Kids and Adults
Night Watch treats the whole family. Whether it is a sick child, an adult with a UTI, a sports injury in a teenager, or STI testing for an adult, our team handles it all under one roof.
At our Aldie location, we also offer care for adolescents and young adults up to 26 years of age, including sexual health services, STI testing, and emotional wellness visits.
On-Site Testing and Treatment No Extra Trips
One of the biggest frustrations with healthcare is being sent somewhere else. Night Watch is built to handle as much as possible in a single visit.
We have on-site X-ray at all three locations, on-site lab testing for strep, flu, COVID, RSV, UTIs, STIs, and more, IV hydration therapy, nebulizer treatment for breathing concerns, and same-day prescriptions. You come in with a problem and leave with a plan.
What Night Watch Can Treat
During Urgent Care Awareness Month, we want every family in Northern Virginia to know what urgent care can actually do. Here is a full picture of what our team handles every day.
Illness Treatment
- Fever evaluation and management
- Ear pain and ear infections
- Strep throat and sore throat with rapid testing on site
- Stomach bugs, vomiting, and nausea
- Respiratory illness including flu, COVID, and RSV
- Sinus infections and congestion
- Allergies and allergic reactions
- Tick bites and Lyme disease evaluation
- UTI diagnosis and treatment
Injury Care
- Cuts and lacerations
- Burns
- Sprains and fractures with on-site X-ray
- Foreign body removal
- Sports injuries
- Scooter and bike injuries
- Concussion evaluation
Diagnostic and On-Site Services
- On-site lab testing for strep, flu, COVID, RSV, UTIs, STIs, and more
- X-ray at all three locations
- IV hydration therapy
- Nebulizer treatment for asthma and breathing flare-ups
- Same-day prescriptions
Additional Services
- Telemedicine visits for when you cannot make it in person
- Physical exams and sports physicals
- STI and STD testing at our Aldie location
- Emotional wellness visits
- Care for adolescents and young adults up to 26 years of age at our Winchester clinic
When to Come to Night Watch Instead of the ER
One of the most common questions we hear is: should I go to the ER or urgent care?
Here is the simple answer.
Go to the ER for: Life-threatening emergencies. Trouble breathing or lips turning blue. Uncontrolled bleeding. Seizures or loss of consciousness. Severe allergic reactions with throat swelling. High fever in a baby under 3 months. Anything that cannot wait even one minute.
Come to Night Watch for: Everything in between. Urgent but not life threatening. Fever, ear infections, strep, injuries, stomach bugs, rashes, tick bites, breathing flare-ups, UTIs, and more. We can handle the in-between moments faster, more affordably, and with less stress than an ER visit.
And if your child needs a higher level of care, we will always tell you and help guide next steps.
Three Locations Across Northern Virginia
Night Watch Urgent Care serves families across Loudoun County, Prince William County, and the Winchester area with three convenient locations.
Aldie / Stone Ridge 42010 Village Center Plaza, Suite 100, Aldie, VA 20105 | (703) 775-4999
Manassas 11700 Sudley Manor Dr, Manassas, VA 20109 | (703) 589-9695
Winchester 2118 Pleasant Valley Road, Winchester, VA 22601 | (540) 545-9999
All three locations are open Monday through Friday 10am to 10pm and Saturday through Sunday 10am to 7pm. Walk-ins always welcome. No appointment needed.
This Month and Every Month
Urgent Care Awareness Month is a reminder that there is a better option between waiting for a Monday appointment and sitting in an ER for four hours.
Night Watch Urgent Care has been that option for Northern Virginia families since 2019. And we are not going anywhere.
If your family has not visited us yet, we hope you will. And if you are already a Night Watch family, thank you for trusting us with your care.
We are here. Every evening. Every weekend. For every in-between moment.
CATEGORY
5/28/2026
POSTED
Night Watch Urgent Care | Sexual Health | Loudoun County & Winchester, VA
Here is something most people do not know. You can feel
completely fine and still have an STI.
No symptoms. No signs. Nothing unusual. Nothing that tells you something is there.
And that is exactly why getting tested matters.
At Night Watch Urgent Care, we offer fast, confidential STI testing with same-day results right here in Loudoun County and Winchester. No appointment needed. No judgment. Just care.
Why Testing Matters
No Symptoms Does Not Mean No Infection
This is the most important thing to understand about STIs. The majority of the most common infection including chlamydia, gonorrhea, and others have no symptoms at all in most people.
No pain. No unusual discharge. No sores. Nothing that signals something is wrong.
That means someone can carry and transmit an infection without ever knowing it. And the only way to truly know your status is to get tested.
Early Detection Changes Everything
When an STI is caught early it is almost always straightforward to treat. A short course of antibiotics. A quick prescription. Done.
Left untreated, the same infections can lead to long-term complications including pelvic inflammatory disease, fertility issues, increased risk of other infections, and more.
The gap between those two outcomes is simply whether or not you got tested.
STI Rates Are Rising in Northern Virginia
STI rates have been increasing nationally and Northern Virginia is no exception.
Reduced testing during and after the pandemic left many infections undetected and untreated. As social activity increased, so did transmission. The result is a community health issue that affects people across all demographics, relationship types, and age groups.
This is not a high-risk group problem. It is a public health reality. And regular screening is simply good healthcare no different from checking your blood pressure or getting a cholesterol panel.
Complete Privacy Always
One of the most common reasons people avoid testing is concern about privacy. We want to be direct about this.
Everything you share with a Night Watch provider is
completely confidential. Our team handles this with professionalism, discretion, and zero judgment — every single day.
No one in your life needs to know you came in. Your health information is yours.
Feeling Nervous Is Completely Normal
Most people feel a little nervous before getting tested. That is normal. That is human.
But here is what we see every day: that nervous feeling lasts about five minutes. The peace of mind that comes after — knowing your status, getting treatment if needed, moving forward with clarity — that lasts a lot longer.
Getting tested is not a sign that something is wrong. It is a sign that you are taking care of yourself.
Our Services
At Night Watch Urgent Care, we offer a full range of sexual health services designed to be fast, private, and accessible.
- STI Testing — Fast, confidential testing with same-day results for the most common sexually transmitted infections.
- Sexual Health Counseling — Judgment-free support and guidance for your health. Whether you have questions about prevention, treatment, or your options, our providers are here to help.
- Prevention and Education — Learn about safer sex practices, PrEP (pre-exposure prophylaxis for HIV prevention), contraception options, and more.
- Treatment and Care — If a test comes back positive, we can treat most infections in the same visit. Same-day prescriptions available.
- Private and Confidential Care — Your privacy is always our priority. Every visit is handled with complete discretion.
We See Patients Up to 26 Years of Age
Quality sexual health care for adolescents and young adults.
We proudly see patients up to 26 years of age at our Winchester clinic conveniently located near Shenandoah University.
Navigating healthcare as a young adult can feel confusing and isolating. You may have aged out of your pediatrician but not feel comfortable at a traditional adult clinic. Night Watch is built for exactly this moment.
Our team provides respectful, age-appropriate care for young adults in a private, non-judgmental environment.
What to Expect at Our Clinics
- Same-day appointments and walk-ins always welcome
- Most insurance accepted
- Confidential and respectful care
- Designed for young adults and adolescents
- Results available same day
- Treatment in the same visit when needed
Taking Care of Your Sexual Health Is Something to Feel Good About
Not something to feel embarrassed about.
Not something to put off.
Sexual health is part of overall health. And you deserve access to care that is fast, private, and built around your real life.
If it has been a while since your last test — or if you have never been tested — this is your sign. We will make it as easy as possible.
Walk in anytime. Rapid STI Testing available on Aldie location. No appointment needed.
CATEGORY
5/18/2026
POSTED
Night Watch Urgent Care | Pediatric Health Blog | May 2026
Locations: Manassas
Your child just threw up. You want to help them feel better. You want to give them something to drink.
But here is where a lot of parents make the situation worse without realizing it.
They either wait too long to give fluids, or they give too much too fast. Both responses can trigger more vomiting, speed up dehydration, and make recovery take longer than it needs to.
There is a better way. It is called the small sips rule, and it is one of the most practical things you can know as a parent.

Why the Stomach Needs Time After Vomiting
When a child vomits, the stomach is irritated and in a heightened state. The muscles that control the stomach are still unsettled, and the body needs a short window to calm down before it can accept anything again.
Giving fluids too quickly, even water, can overwhelm a sensitive stomach and trigger another vomiting episode. This is not a sign that your child is getting sicker. It is simply the stomach rejecting too much too soon.
The small sips rule exists to work with the body, not against it.
The Small Sips Rule: Step by Step
Step 1: Wait 15 to 20 minutes after the last vomiting episode before offering anything.
This is the part most parents skip. It feels counterintuitive to wait when your child is uncomfortable and asking for water. But giving fluids immediately after vomiting is one of the most common reasons vomiting continues.
Step 2: Start with one teaspoon every 5 minutes.
One teaspoon. That is it. Not a cup. Not a few gulps. Just one teaspoon, offered slowly, every 5 minutes.
A teaspoon is about 5 milliliters. You can use a small medicine syringe if your child will not sip from a cup or spoon.
Step 3: If they keep it down for 30 minutes, slowly increase the amount.
After 30 minutes of keeping small sips down, you can move to a tablespoon every few minutes. Then gradually work up to small sips on demand.
The goal is slow and steady. Do not rush this process even if your child says they are thirsty. The stomach needs time.
What to Give and What to Avoid
Not all fluids are equal when it comes to vomiting and dehydration recovery.
Best options:
- Pedialyte or oral rehydration solutions (ORS)
- Water, if ORS is not available
- Frozen Pedialyte pops or ice chips
- Clear broth in small amounts once vomiting has settled
What to avoid:
- Juice and sports drinks. The high sugar content can irritate the gut and worsen diarrhea.
- Milk or dairy. Can be harder to digest and may increase nausea.
- Carbonated drinks. The bubbles can make nausea worse.
- Large amounts of plain water all at once. In young children, too much plain water without electrolytes can cause an imbalance.
When Is It Safe to Introduce Food Again?
Food is not the priority right away. Hydration comes first.
Once your child has kept fluids down for several hours and vomiting has stopped or significantly slowed, you can slowly reintroduce bland foods.
Think plain crackers, toast, banana, or plain rice. Small amounts. Let your child guide how much they want.
Do not push food if they are not interested. Appetite coming back slowly after a stomach illness is completely normal and expected.
Signs of Dehydration to Watch For
This is the most important part of managing vomiting at home. Dehydration in children can develop faster than most parents expect, especially in younger kids.
Watch for these signs:
- Dry or sticky mouth and lips
- No tears when crying
- No urine in 6 to 8 hours or significantly fewer wet diapers
- Sunken eyes
- Unusual sleepiness or low energy
- Pale or mottled skin
If your child is showing more than one of these signs and is not keeping fluids down, it is time to get them evaluated. IV fluids may be needed to catch up on what has been lost.
When to Come In
Managing vomiting at home with the small sips rule works well for most cases. But there are situations that should not be waited out.
Come in to see us if:
- Vomiting has not slowed after 6 to 8 hours and your child cannot keep anything down
- You are seeing clear signs of dehydration
- Your child is under 1 year old and has vomited more than twice
- There is blood or green color in the vomit
- Vomiting is accompanied by severe belly pain, especially on the right side
- Your child had a head injury before the vomiting started
- Something just does not feel right
That last one matters. You know your child. If their behavior seems off, they are unusually pale or limp, or your gut is telling you something is wrong, come in. We would rather see them and reassure you than have you managing something serious at home.
We Are Here When You Need Us
At Night Watch Urgent Care, we see children with vomiting and dehydration every day across our clinics in Northern Virginia. Whether it is a stomach bug, norovirus, or something else, we can evaluate your child quickly and help you get on the right path.
We offer IV fluids on site when needed, and our team will give you a clear plan for home care before you leave.
Open late every weekday and every weekend. Walk-ins always welcome.
CATEGORY
5/09/2026
POSTED
Seasonal allergies are one of the most common conditions we see in children — especially this time of year.
Across our clinics in Aldie (Stone Ridge), Manassas, and Winchester, we’re seeing more kids come in with congestion, sneezing, itchy eyes, and symptoms that seem to linger longer than expected.
For many families, it can feel confusing. Symptoms come and go, don’t fully resolve, and often look like a cold.To help you better understand what’s going on, here are five things many parents don’t realize about kids’ seasonal allergies.

1. Allergies can trigger asthma flare-ups
If your child has asthma, there’s a strong chance that allergies are playing a role.
In fact, many children with asthma also have environmental allergies that can trigger symptoms like coughing, wheezing, and shortness of breath. This is especially common during seasonal changes when pollen levels are higher.
That’s why breathing symptoms may seem worse when allergy symptoms are also present — and why early management matters.
2. Waiting for symptoms to start can make them harder to control
Many allergy treatments are designed to prevent symptoms, not just treat them after they begin.
If your child tends to have seasonal allergies every year, starting treatment early — before symptoms peak — can help reduce how severe they become.
This is something many parents don’t realize until symptoms are already in full swing.
3. Not all home remedies work the way you think
You may have heard that local honey can help with allergies.
While honey is safe for children over 1 year old and can soothe a cough, there’s no consistent evidence that it prevents or treats seasonal allergies.
It’s fine to use as a comfort measure — just not as a primary solution for allergy symptoms.
4. Pollen counts don’t tell the whole story
Checking the pollen count can be helpful, but it doesn’t always explain your child’s symptoms.
Different children react to different types of pollen — like tree, grass, or weed pollen — and most reports only show a general overall level.
That’s why some kids may have significant symptoms even when the pollen count doesn’t seem especially high.
5. There are more treatment options than you might think
For some children — especially those with persistent or more severe symptoms — there are additional options beyond basic allergy medications.
These may include targeted treatments or allergy-specific therapies, depending on your child’s age, symptoms, and triggers.
The right approach varies for each child, which is why getting the right evaluation can make a difference.
What this means for parents
If your child’s symptoms are lingering, worsening, or not responding the way you expected, you’re not alone.
We’re seeing a lot of this right now.
Sometimes it’s straightforward seasonal allergies. Other times, symptoms may overlap with other conditions.
Either way, getting clarity can help guide the right next steps and help your child feel better sooner.
Allergy care at Night Watch Urgent Care
At Night Watch Urgent Care, we evaluate and treat seasonal allergies and related symptoms in children across Northern Virginia.
We help determine what’s causing your child’s symptoms and recommend the next steps — whether that’s supportive care, symptom management, or further evaluation.We’re open every day, including evenings and weekends, so you don’t have to wait while symptoms linger.
Seasonal allergies can be frustrating — especially when symptoms don’t go away as expected.
If you’re unsure what’s normal or what to do next, it’s always okay to have your child evaluated.
CATEGORY
5/01/2026
POSTED
A quick update from our clinics
Allergies are everywhere right now.
Over the past week, we’ve been seeing a steady flow of kids coming into our clinics in Aldie (Stone Ridge), Manassas, and Winchester with the same pattern of symptoms.
It’s not the typical “gets better in a few days” kind of illness.
It lingers.
And that’s what’s making it confusing for a lot of families.

What we’re seeing in clinic
Most kids we’re seeing right now are coming in with:
- Congestion that won’t go away
- Frequent sneezing
- Runny nose that keeps coming back
- Itchy or watery eyes
- Red, irritated eyes (often mistaken for pink eye)
- A cough that’s worse at night
For many parents, it starts off feeling like a simple cold. But after a few days, it doesn’t improve the way they expected.
Instead of getting better, symptoms just stay — or fluctuate throughout the day.
That’s been one of the biggest patterns we’re seeing.
Why symptoms are worse right now
This is very typical for this time of year in Northern Virginia.
Pollen levels are rising, the weather keeps shifting, and allergens are more active — especially outdoors.
Even children who don’t usually have strong allergies can start showing symptoms when exposure increases.
And because allergy symptoms can overlap with colds, it’s easy to misread what’s going on.
When it’s more likely allergies
There’s no single symptom that confirms it, but there are a few patterns we’re seeing consistently right now.
Symptoms that linger beyond a few days, come and go, or seem worse in the morning or after being outside are often allergy-related.
Itching is another big clue — especially itchy eyes, nose, or throat — which isn’t as common with viral illnesses.
Most of the time, the discharge is also clear rather than thick, and kids may seem uncomfortable but otherwise okay.
What to do next
Not every case needs immediate treatment, but getting clarity can help a lot.
If your child’s symptoms aren’t improving, are affecting sleep, or just don’t feel typical for them, it’s reasonable to have them evaluated.
Sometimes it’s simply confirming that it’s allergies and guiding you on what will help. Other times, it helps rule out something else.
Either way, it takes the guesswork out of it.
Allergy care at Night Watch Urgent Care
At Night Watch Urgent Care, we’re seeing and treating seasonal allergies in children every day right now.
We help families understand what’s causing their child’s symptoms and recommend the right next steps — whether that’s supportive care, allergy management, or further evaluation.We’re open every day, including evenings and weekends, so you don’t have to wait while symptoms linger.
CATEGORY
4/19/2026
POSTED
exacerbations — often triggered by recent weather changes.

Across Aldie (Stone Ridge), Manassas, and Winchester, more families are coming in with children experiencing coughing, wheezing, and breathing difficulties. In many cases, symptoms started mild but progressed quickly over a few days.
Seasonal transitions in Northern Virginia can make asthma harder to control — especially when temperature shifts, allergens, and viruses all overlap.
Why Weather Changes Trigger Asthma
Asthma affects the airways, making them more sensitive to environmental changes. When the weather shifts, the airways can become irritated and inflamed.
Cold air can cause the airways to tighten, while warmer conditions may increase exposure to allergens like pollen and mold. Rapid temperature changes — such as warm days followed by cool evenings — can also make it harder for children’s bodies to adjust.
At the same time, seasonal changes often bring more viral illnesses, which can further worsen asthma symptoms.
What Asthma Flare-Ups Can Look Like
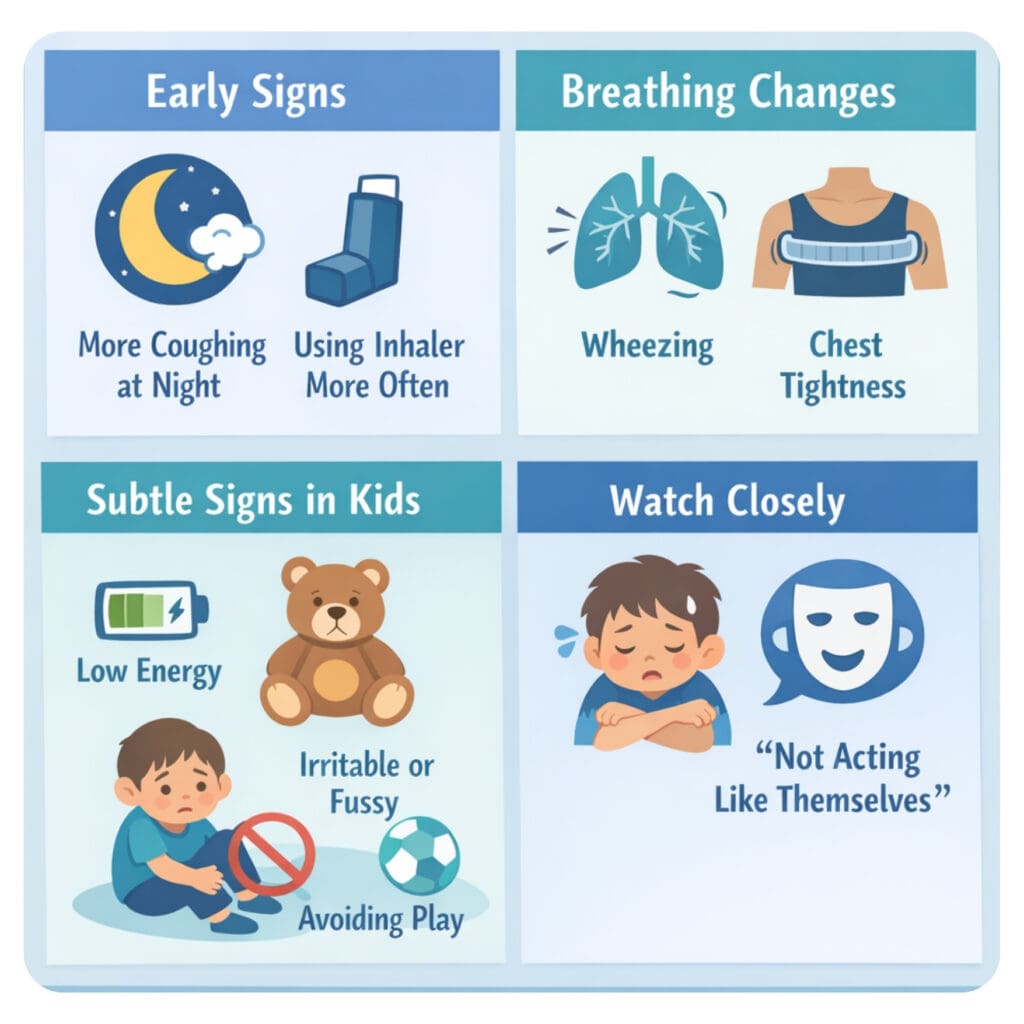
Asthma flare-ups don’t always start suddenly. Many begin with subtle symptoms that can be easy to overlook.
You may notice your child coughing more frequently, especially at night, or needing their inhaler more often than usual. Some children develop wheezing, which sounds like a whistling noise when breathing, while others may complain of chest tightness.
In younger children, symptoms may show up as low energy, irritability, or avoiding physical activity. Even small changes — like getting winded more easily or “not acting like themselves” — can be early signs that their breathing is affected.
When to Have Your Child Evaluated
If your child’s symptoms are not improving with home care or their usual medications, it may be time to have them evaluated.
At Night Watch Urgent Care, we regularly see children with asthma flare-ups who benefit from same-day care and early treatment. Addressing symptoms early can help prevent them from becoming more severe.
If your child is needing their inhaler more frequently, experiencing worsening cough, or having difficulty with normal activities, it’s best not to wait.
When Asthma Symptoms Become Urgent
Some symptoms require immediate medical attention.
If your child is breathing rapidly, using extra muscles to breathe (such as ribs pulling in or nostrils flaring), struggling to speak, or showing signs like bluish lips or unusual drowsiness, they should be taken to the emergency room right away.
These are signs of significant respiratory distress and should not be delayed.
Asthma Care at Night Watch Urgent Care
At Night Watch Urgent Care, we provide evaluation and treatment for asthma exacerbations and breathing concerns in children across Northern Virginia.
Our clinics offer:
- Same-day urgent care visits
- Breathing treatments, including nebulizer therapy
- On-site evaluation and monitoring
We’re open every day, including evenings and weekends, so families can access care when symptoms begin — not hours later.
Asthma flare-ups during weather changes are common — especially this time of year — but they can escalate quickly if not addressed early.
If your child’s symptoms are changing, worsening, or not improving, it’s always okay to have them checked.
CATEGORY
4/12/2026
POSTED
As the weather warms up in Northern Virginia, families are spending more time outdoors — at parks, trails, sports fields, and even in their own backyards. But with that increase in outdoor activity comes a higher risk of tick bites and Lyme disease.
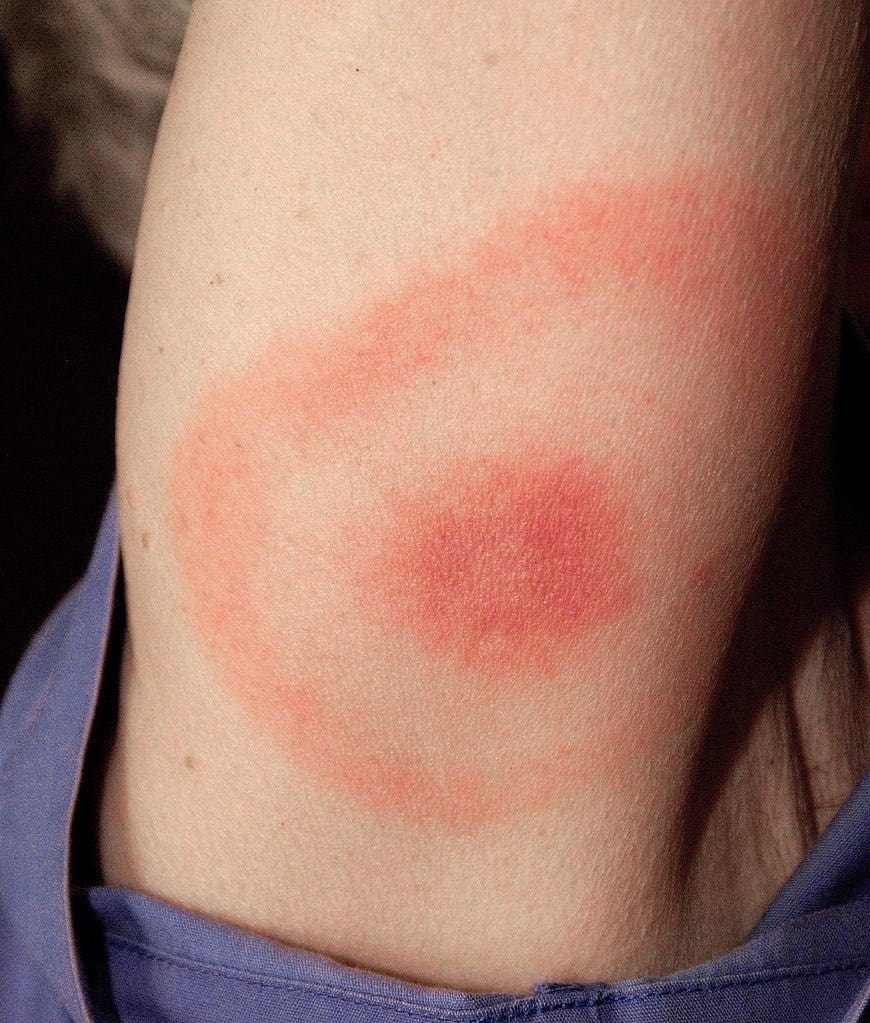
According to a recent Loudoun County health update, tick season is highest from May through October, and our area continues to report some of the highest Lyme disease rates in Northern Virginia.
Understanding how to prevent tick bites — and recognizing early symptoms — can help protect your family during the months ahead.
What Is Lyme Disease?
Lyme disease is a bacterial infection spread through the bite of an infected blacklegged tick (also known as a deer tick).
These ticks are commonly found in wooded areas, tall grass, and brush, making everyday outdoor activities a potential source of exposure.
Lyme disease is the most common tick-borne illness in Loudoun County, but other tick-related illnesses can also occur, which is why awareness is important.
Signs and Symptoms of Lyme Disease
One of the challenges with Lyme disease is that symptoms don’t always appear right away — and many people don’t remember being bitten by a tick.
Early symptoms may include:
- Fever or chills
- Fatigue
- Headaches
- Muscle or joint pain
- A “bull’s-eye” rash (erythema migrans)
These symptoms can feel similar to a viral illness, which is why they’re sometimes overlooked.
If untreated, Lyme disease can affect the joints, heart, and nervous system, making early recognition and treatment especially important.
When Does Lyme Disease Spread?
Ticks can be active year-round, but risk is highest during warmer months.
In general, Lyme disease transmission usually requires a tick to be attached for at least 24 hours, although other tick-borne illnesses may spread more quickly.
Because tick bites are often painless and easy to miss, regular checks after outdoor activity are essential.
How to Prevent Tick Bites
Simple prevention steps can significantly reduce your risk of Lyme disease:
- Use insect repellent with 20% DEET or EPA-approved ingredients
- Wear long sleeves and long pants when outdoors
- Avoid tall grass and stay in the center of trails
- Choose light-colored clothing to spot ticks more easily
- Check your child’s skin, scalp, and clothing after outdoor activities
- Shower within two hours of coming indoors
- Place clothes in the dryer on high heat after outdoor exposure
- Remove ticks promptly with fine-tipped tweezers

These small habits can help protect both children and adults during peak tick season.
When Should You Get Checked?
You should consider medical evaluation if your child or family member has:
- A rash after outdoor exposure
- Flu-like symptoms during tick season
- Unexplained fatigue or joint pain
- A known or suspected tick bite
Even if symptoms seem mild, early evaluation can help guide next steps and prevent complications.
Lyme Disease Care in Loudoun County and Northern Virginia
At Night Watch Urgent Care, we evaluate tick bites, rashes, and symptoms of Lyme disease with same-day care across Northern Virginia.
Our providers understand that early symptoms can be subtle, and we’re here to help you determine whether further evaluation or treatment is needed.
We’re open evenings and weekends, so you don’t have to wait to get your child checked.
CATEGORY
4/06/2026
POSTED
Respiratory symptoms in children are becoming more common across the United States, especially during seasonal transitions. Many healthcare providers are reporting an increase in cough, wheezing, and asthma flare-ups in children, often triggered by a mix of viruses, allergies, and weather changes.
We’re seeing the same pattern locally at Night Watch Urgent Care in Stone Ridge (Aldie), Manassas, and Winchester, where more families are coming in with concerns about their child’s breathing.
For many children, symptoms begin mild — a simple cough or slight fatigue — but can progress quickly if not monitored closely.

Common Breathing Symptoms in Kids
Breathing problems in children don’t always look severe at first, which can make it difficult for parents to know when to be concerned.
A frequent or worsening cough, especially at night, is often one of the earliest signs. Some children may start needing their inhaler more often than usual, while others develop a wheezing or whistling sound when breathing, which can indicate narrowed airways.
In other cases, children may complain of chest tightness or appear more tired than usual. Subtle changes — like avoiding play, getting winded easily, or simply “not acting like themselves” — can be early indicators that their breathing is affected.
Recognizing these signs early can help prevent symptoms from worsening.

When to Bring Your Child to Urgent Care
If your child’s symptoms are not improving with home care or their usual medications, it may be time to have them evaluated.
At Night Watch Urgent Care, we regularly treat children with asthma flare-ups, persistent cough, and breathing difficulties who benefit from same-day care. Early evaluation allows providers to assess your child’s breathing, adjust treatment if needed, and help prevent symptoms from escalating.
Seeking care sooner rather than later can reduce the likelihood of needing emergency treatment.
When Breathing Symptoms Become Urgent
Some symptoms require immediate medical attention and should not be delayed.
If your child is breathing rapidly, struggling to catch their breath, using extra muscles to breathe (such as ribs pulling in or nostrils flaring), or having difficulty speaking, they should be taken to the emergency room right away.
Other warning signs include bluish lips or face, extreme fatigue, or unusual drowsiness. These may indicate serious respiratory distress and require urgent care.
Pediatric Urgent Care for Breathing Issues in Northern Virginia
At Night Watch Urgent Care, we provide evaluation and treatment for asthma flare-ups, wheezing, and respiratory symptoms in children across Northern Virginia.
Our clinics offer:
- Same-day urgent care visits
- Breathing treatments, including nebulizer therapy
- On-site evaluation and monitoring
We’re open every day, including evenings and weekends, so families can access care when symptoms start — not hours later.
CATEGORY
3/30/2026
POSTED
6 Things Night Watch Urgent Care Does Differently
When your child gets sick or injured, one of the hardest decisions parents face is where to go. Should you wait for your pediatrician? Head to the emergency room? Or look for an urgent care that actually understands pediatric needs?
At Night Watch Urgent Care, we’ve built our clinics around what families truly need: convenience, clarity, and care that fits real life.
Here are six ways we do things differently.
1. Pediatric Urgent Care Designed for Real Life
We are not just an urgent care clinic — we are a pediatric-focused environment designed to make children feel comfortable and supported.
From common illnesses like fevers and coughs to injuries that happen during play or sports, our approach centers on both medical care and the overall experience for families.
2. Open Late and on Weekends
Illness doesn’t follow office hours, and neither do we.
⏰ Hours:
Monday–Friday: 10 AM – 10 PM
Saturday–Sunday: 10 AM – 7 PM
Whether symptoms start after school or worsen at night, families have access to care when they actually need it.
3. We Treat More Than You Might Expect
Many parents are surprised by the range of conditions we manage.
We regularly treat:
• Flu symptoms and respiratory illnesses
• Ear infections and sore throats
• Minor fractures, sprains, and sports injuries
• Cuts that require stitches
• Rashes and allergic reactions
• Dehydration and stomach illnesses
This means fewer referrals and fewer stops for care.
4. On-Site X-Rays and Testing
One of the biggest advantages of visiting Night Watch Urgent Care is access to immediate diagnostics.
With on-site X-rays and testing, we can:
• Confirm fractures
• Evaluate injuries
• Diagnose infections
• Provide same-visit treatment plans
Families don’t have to wait days for answers or travel to multiple locations.
5. Helping Families Avoid Unnecessary ER Visits
Emergency rooms are essential for serious, life-threatening conditions — but many situations fall into a gray area.
When it’s urgent but not an emergency, urgent care is often the right choice.
At Night Watch, we provide timely evaluation and treatment so families can avoid long ER wait times and higher costs when appropriate.
6. Care for Both Kids and Adults at Stone Ridge
📍 Stone Ridge Location
In addition to pediatric care, this location also treats adults.
This makes it easier for families to receive care together, especially when multiple members are feeling unwell or need evaluation at the same time.

Convenient Care Across Northern Virginia
Night Watch Urgent Care serves families across:
• Manassas
• Winchester
• Aldie / Stone Ridge
With extended hours, comprehensive services, and a family-centered approach, we are here when care can’t wait.
When to Visit Night Watch Urgent Care
If your child is sick, injured, or something simply doesn’t feel right, it’s always okay to seek care.
Having access to a trusted urgent care can make these moments less stressful and more manageable.
We are open late and available on weekends to support your family’s needs.
Care should be accessible, efficient, and built around real life — and that’s exactly what we aim to provide.
CATEGORY
3/23/2026
POSTED
the past seven years, Night Watch Urgent Care has been proud to serve families across Northern Virginia by providing trusted pediatric urgent care when children need it most.
What began as a mission to make healthcare more accessible for families has grown into a reliable resource for parents looking for evening and weekend pediatric care outside traditional office hours.
Over the years, our clinics have helped thousands of families navigate everything from late-night fevers and sudden illnesses to minor injuries and unexpected health concerns.

Supporting Families When It Matters Most
Children rarely get sick at convenient times. Many parents find themselves searching for urgent care for kids near them late at night or on weekends when their pediatrician’s office is closed.
That is exactly why Night Watch Urgent Care exists.
Our team provides accessible pediatric urgent care services, helping families receive timely medical attention without the long wait times often associated with emergency rooms.
Common reasons families visit our clinics include:
• Fevers and viral illnesses
• Ear infections
• Cough, wheezing, and breathing concerns
• Minor injuries and fractures
• Rashes and allergic reactions
• Vomiting and dehydration
• Concussions and head injuries
Every visit is an opportunity to provide reassurance, answers, and compassionate care for both children and parents.
Pediatric Care That Focuses on Families
At Night Watch Urgent Care, pediatric care goes beyond treating symptoms. We focus on creating an environment where children feel comfortable and parents feel supported.
Our providers understand that when a child is sick, families need more than just medical treatment. They need guidance, clear communication, and confidence that they are making the right decisions for their child’s health.
For the past seven years, families have trusted our team to provide that care, and we are deeply grateful for the opportunity to serve our community.
Thank You for Trusting Us
Reaching this seven-year milestone would not have been possible without the families who have chosen Night Watch Urgent Care for their children’s healthcare needs.
We are incredibly thankful to the parents, caregivers, and children who have walked through our doors, called us for guidance, or trusted us during difficult moments.
Serving this community is an honor, and we look forward to continuing to support the health and well-being of families for many years to come.
Pediatric Urgent Care When You Need It
Night Watch Urgent Care provides convenient pediatric urgent care with evening and weekend availability, making it easier for families to get care when traditional offices are closed.
Walk-ins are welcome.
Stone Ridge (Aldie, VA)
42010 Village Center Plaza, Ste 100
(703) 775-4999
Winchester, VA
2118 Pleasant Valley Rd
(540) 545-9999
Manassas, VA
11700 Sudley Manor Dr
(703) 589-9695
If you are searching for pediatric urgent care near you, our team is here to help.
Share Your Experience
If Night Watch Urgent Care has cared for your family over the years, we would love to hear your story. Your feedback helps us continue improving and supporting families across our community.
Thank you for being part of our journey.
CATEGORY
3/10/2026